In June 2017, I was a 63-year-old runner, long-distance open-water swimmer, hiker, hobby photographer, and middle-school science journal editor. I had been weight-training for 15 years. Had I been born decades later, I would have been diagnosed as hyperactive. I often thought that a hyperactive child is frustrating for adults, but being a hyperactive adult is great because you have abundant energy.
In July 2017, I experienced an ischemic stroke in my right cerebral hemisphere. I was affected on my left side following my stroke and I am left-dominant. At the time of my stroke, I did not understand the severity of my injury. I was optimistic because my body had never let me down. I was sure I would be back to my active self within a few months, even though a physician friend told me I would spend a year in recovery, if not longer. I began reading about stroke recovery while in inpatient rehab. Slowly, I began to understand that my condition was worse than I thought, and I had a long road to travel. I never doubted, however, that I would recover. I just needed to figure out how to do it.
Painting as a Healing Art
I contemplated painting as a hobby just before the first anniversary of my stroke, since so many of my favorite more rigorous activities were restricted by the stroke’s effects. I had painted years before, although photography had been my more recent medium of choice. I probably would have focused on photography as a hobby, except that my mobility was insufficient to walk where I like to take photos and my left hand and wrist would not move adequately to make photography a practical hobby at that point in my ongoing recovery.
When I told my Emory neurologist, Dr. Samir Belagaje of my plan to begin painting, he advised, “Paint with your left hand!” I realized the wisdom in this suggestion. Painting with my affected hand would provide needed fine motor movement for rehabilitation purposes. I had rejected other standard hand therapies, such as putting lids on jars, and even repetitive computer-based therapy games. I found them boring. I knew I did not need to spend more time in front of a screen. I wanted to be creative.
All the images in this essay were created following my stroke. Using my left hand to draw and paint has facilitated my hand’s and wrist’s fine movement, although recovery remains slow, even 18 months past my first painting (2.5 years post-stroke). Each image in this essay is accompanied by a short narrative that explains its significance as a physical therapy. At the beginning, I approached each project with its specific movement requirements in mind, exercising different arm, hand, and wrist muscles as required by the medium.
This narrative, therefore, describes an exploration of my brain’s neuroplasticity, my struggle for fine motor control in my affected hand and wrist, and my journey creating art, no matter the result.
My Journey
 July 2018: Boat in Loch Harray, Orkney Islands, Scotland, tempera
July 2018: Boat in Loch Harray, Orkney Islands, Scotland, tempera
My husband Ken and I travel to Scotland every other year. In 2017, we visited Scotland’s Orkney Islands. This boat had been pulled onto Orkney’s Loch Harray shore, just a few hundred feet from our hotel. I have an affection for row boats, having spent many hours in my teen years rowing one like this. I took a photograph of the boat and painted from the photograph. The photograph was taken about 2 months before my stroke in 2017.
This was my first painting after my stroke, and I finished it just one day shy of my first stroke anniversary. I decided to use tempera paint because it is inexpensive and easy to use. I had no idea what to expect. My main goal was improved movement, not great art. Although the painting is rough, I was surprised that I had any hand control at all.
 September 2018: St. Clements Church, Isle of Harris, Scotland, tempera
September 2018: St. Clements Church, Isle of Harris, Scotland, tempera
This painting was done from a photograph I took in 2015 on the southern tip of the Isle of Harris, Scotland. This is St. Clement’s Church, built in the late 1400s or early 1500s. Ken and I have visited this church at least four times, and its exterior architecture and interior sanctity have always captured my affection and provided inspiration.
With this painting, I discovered that I could be more successful at painting if I dabbed paint on the paper. This was an important discovery because my wrist would not bend, and brush strokes, therefore, were challenging.
 November 2018: Moonlight Through Church Window, tempera
November 2018: Moonlight Through Church Window, tempera
This window is in a corner of our bedroom. Early one August morning in 2018, I woke up to see light from the setting full moon flowing through the glass. I got up, took a photograph, and painted this painting from that photograph.
This was further experimentation with the dabbing technique first tried in September. Dabbing gave me a way to paint without using my wrist, which still would not extend. I also found it hard to hold the brush. Dabbing gave me ample opportunity to rest between “dabs” as needed, but I dropped the brush many times and had to cover up unwanted paint blobs.
 October 2018: Tallassee Oak, charcoal and pastel
October 2018: Tallassee Oak, charcoal and pastel
This majestic white oak is growing beside my house. It is hundreds of years old, and it takes four people holding hands to surround the trunk.
Dr. Rich Panico, my meditation teacher and an artist, recommended that I try charcoal on large paper to give my entire arm an opportunity to practice control. I decided to add pastel chalk because I like to use color. I found it difficult to control charcoal and pastels. I dropped (and broke) many pieces of chalk while drawing this tree. The trunk is lighter at the top because the evening sun was illuminating the upper part of the tree. All I could do was scratch and scribble; drawing small shapes was out of the question.
 January 2019: Southern Utah, colored pencil
January 2019: Southern Utah, colored pencil
This drawing was from a photograph I took in 2014 while Ken and I were traveling in Utah.
I felt that my wrist needed an opportunity to practice extension, so I decided to try colored pencils. I had never used colored pencils before. In this effort, I found it difficult to press hard on the paper, extend my wrist to complete the pencil lines, hold the pencil, and maintain control. This drawing exhausted me. You can imagine how pencil lines require wrist flexion and extension, and perhaps understand the challenge I faced. This drawing experience, in spite of its difficulty, was much more rewarding to me than handling jar lids or folding clothes.

 January 2019: South Harris Beach, Scotland, colored pencil and tempera
January 2019: South Harris Beach, Scotland, colored pencil and tempera
The Outer Hebridean Isle of Harris is known for its tweed and its white sand beaches. These two drawings were done from the same photograph, most likely taken in 2013.
Have you ever tried things that just did not work? Emboldened by my colored-pencil experience, I tried another pencil drawing and became so frustrated that I allowed my right hand to help. The result was sub-par. I tried the same scene with tempera, with an equally undesirable result. At least my left hand had more practice. I love water landscapes, but this experience taught me how hard water is to capture in drawings and paintings.
 February 2019: Tuckasegee River, Nikon 7200 DSLR
February 2019: Tuckasegee River, Nikon 7200 DSLR
The Tuckasegee River is in the mountains of Western North Carolina. It is one of my favorite rivers to photograph, since the water is clear and therefore reflects colors and light in a wide variety of delightful ways.
Prior to my stroke, one of my favorite hobbies was photography. I particularly like to photograph the surface of natural waters. My stroke inhibited my using my Nikon DSLR in three ways: 1) I could not turn the zoom lens with my left wrist; 2) the camera was too heavy to easily use with one hand; 3) I could not walk or move into proper position for my desired photo, which was often in hard-to-reach natural settings. This photograph marks the first time I was able to move into a position that enabled me to get the photograph I wanted. The riverbank was just a small downhill (and grassy at that!), but it was an important accomplishment for me.
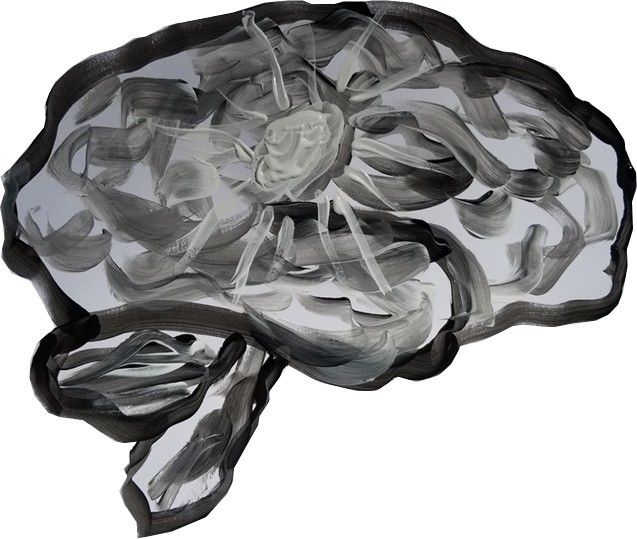
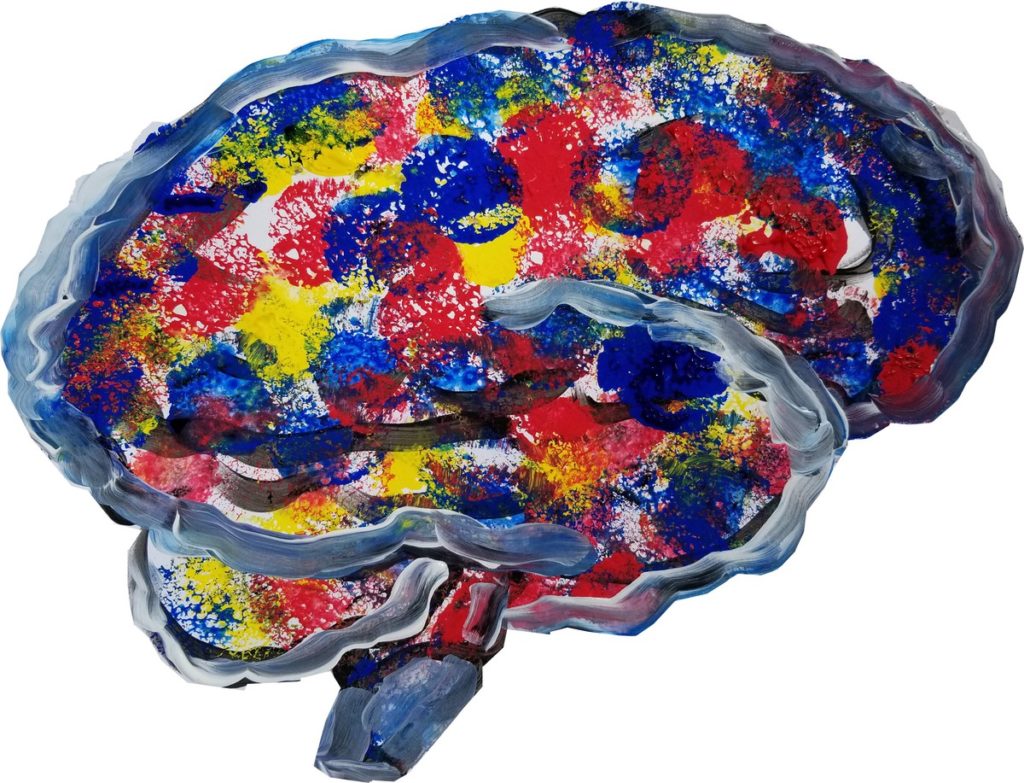 March 2019: Brain Stroke/Brush Stroke, tempera
March 2019: Brain Stroke/Brush Stroke, tempera
I volunteered for a clinical trial at Emory University in early 2019. I discussed my painting projects with Dr. Trisha Kesar, the principal investigator. Dr. Kesar showed me a painting she had done of a human brain. It was lovely and I was inspired. While preparing for a presentation about my stroke recovery journey, I decided to quickly paint my own brain with its ischemic stroke and its subsequent recovery process to use on the cover slide.
Immediately after finishing the paintings, I felt an almost imperceptible improvement in my overall condition. Describing such a small improvement is difficult. Did I just imagine it? The effect was not tangible. The best way to describe it was as knowledge of a small shift toward improvement in my brain and body. That experience of improvement inspired me to try some additional “self-portraits,” with a different twist.
 April 2019: Brain to Deltoid Connection, charcoal and pastel
April 2019: Brain to Deltoid Connection, charcoal and pastel
After reflecting on what I felt was a small shift resulting from my brain paintings (Brain Stroke/Brush Stroke), I wondered if drawing the brain-muscle connection would have any effect on my recovery. I knew that visualization was recommended as a stroke-recovery therapy (so of course I tried it). Visualization, as I understood it, involved imagining a desired movement in detail. I, for example, imagined in detail swimming or running. This imagining experience was entirely internal and focused on movement. Enlisting my eyes, I reasoned, would enhance the chances of facilitating the desired brain-muscle communication, literally showing my brain what I wanted it to do. I know that people often learn by watching and/or by doing. I thought that I would combine these known learning techniques for stroke recovery, taking visualization a step further and closer to the genesis of movement.
This drawing was my first attempt to visually show my brain what I wanted it to do. In this drawing, I wanted to improve my brain-to-deltoid nerve connection. Prior to completing this drawing, my deltoid was tested using electromyography (EMG) and found to lack innervation. The doctor who did the EMG told me that I would never have use of my deltoid again. I could lift my left arm only about 10 degrees to the side. I believe the drawing helped to reestablish or support the nerve reconnection. Within a few days of completing this drawing, I was able to lift my arm to about 45 degrees using the deltoid. Note that the connection I’ve drawn is between the right brain hemisphere and my left deltoid. After completing a few more of these brain-to-muscle drawings, I named this technique autophysioartistry, or APA.
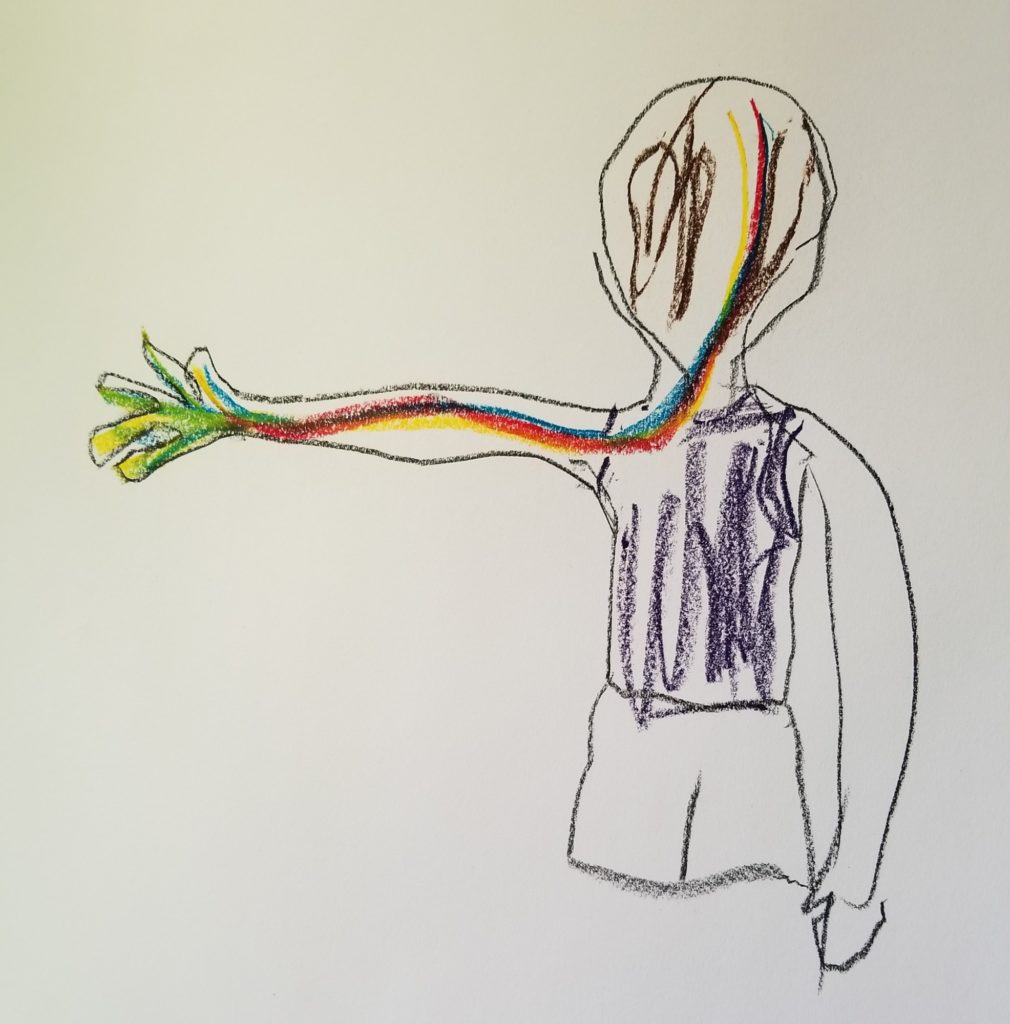 April 2019: Brain to Hand Connection, charcoal and pastel
April 2019: Brain to Hand Connection, charcoal and pastel
Following the deltoid experience, I drew three more APA drawings using a pencil. I “knew” that my mobility was improving as I completed more APA drawings. The deltoid example was dramatic and measurable, but subsequent brain-to-muscle connections were not as easily measured.
After completing the trio of APA pencil drawings, I determined that pencil lines were too timid. I tried another charcoal and pastel drawing. This drawing feels like it has power to convey to my brain what I want it to do.
 May 2019: Woodland Ransome Wildflowers, Lake District, England, Nikon DSLR 7200
May 2019: Woodland Ransome Wildflowers, Lake District, England, Nikon DSLR 7200
In May and June 2019, Ken and I traveled to the UK. On the way to Scotland, we traveled through England’s Lake District. As we drove north, I noticed a blanket of white on the forest floor.
Getting this photograph required my walking through thick waist-high vegetation while holding my Nikon camera above the vegetation. Another first in my recovery journey! I would have not tried the short but weedy trek if it had not been for the lovely landscape and my desire to photograph it. Taking this photograph made me feel like I was making progress toward my pre-stroke self.
 June 2019: Village Bay, Hirta, St. Kilda, Scotland, Nikon DSLR 7200
June 2019: Village Bay, Hirta, St. Kilda, Scotland, Nikon DSLR 7200
During our Scottish travels, Ken and I visited St. Kilda archipelago 50 miles off the Scottish west coast. St. Kilda is only accessible to visitors who endure a 3-hour boat trip across the often-turbulent north Atlantic Ocean. Ours was a small boat that accommodated 12 passengers with an open area in the back of the boat. As we left St. Kilda, I saw these lovely colors and wanted to capture them, even though the boat was accelerating and was somewhat unsteady.
I needed to use both hands to get the shot from the back of the boat. Getting this photograph required balance and quickness.
 July 2019: Kingfisher Creek, Olympus Tough (camera)
July 2019: Kingfisher Creek, Olympus Tough (camera)
Kingfisher Creek marks our property line in Georgia. The creek is located down a series of old cotton terraces through what is now mature forest. The way is relatively steep with no trail. The walk is pleasant, but it is a difficult task for a person relearning to walk. I love this creek and have felt solace for more than 35 years sitting along its banks.
On this morning, I walked alone to the creek for peace, exercise, practice, and to take photographs. Getting to the rocks at the water’s edge required my maneuvering down a steep but short bank. I suppose I risked falling but I used my walking stick for support. This experience gave me confidence and boosted my feeling of independence.
 July 2019: Purple Mountains, watercolor pencil
July 2019: Purple Mountains, watercolor pencil
In early spring 2019, a salesperson at my local artist-supply store suggested I try watercolor as a part of my art physical therapy. I had never used watercolor and was reluctant to try it, given my lack of control and unfamiliarity with how to paint with watercolor. Then coincidentally, prior to joining us during our UK vacation in June 2019, friends had visited a pencil museum and were given four watercolor pencils as a parting memento from the museum. They gave their pencils to me. I decided to give the pencils a try, and painted this scene using the four colors. The salesperson was correct about watercolor’s physical therapy benefits—or at least watercolor pencils’ benefits.
The initial pencil strokes required wrist movement like that with colored pencils, and the followup brush strokes required a more fluid, whole-hand motion. Only having four colors required me to vary the pressure of the pencil stroke to create color variations in the wheat. I found that I was only marginally successful using watercolor pencils. They are a medium that might require expert instruction.
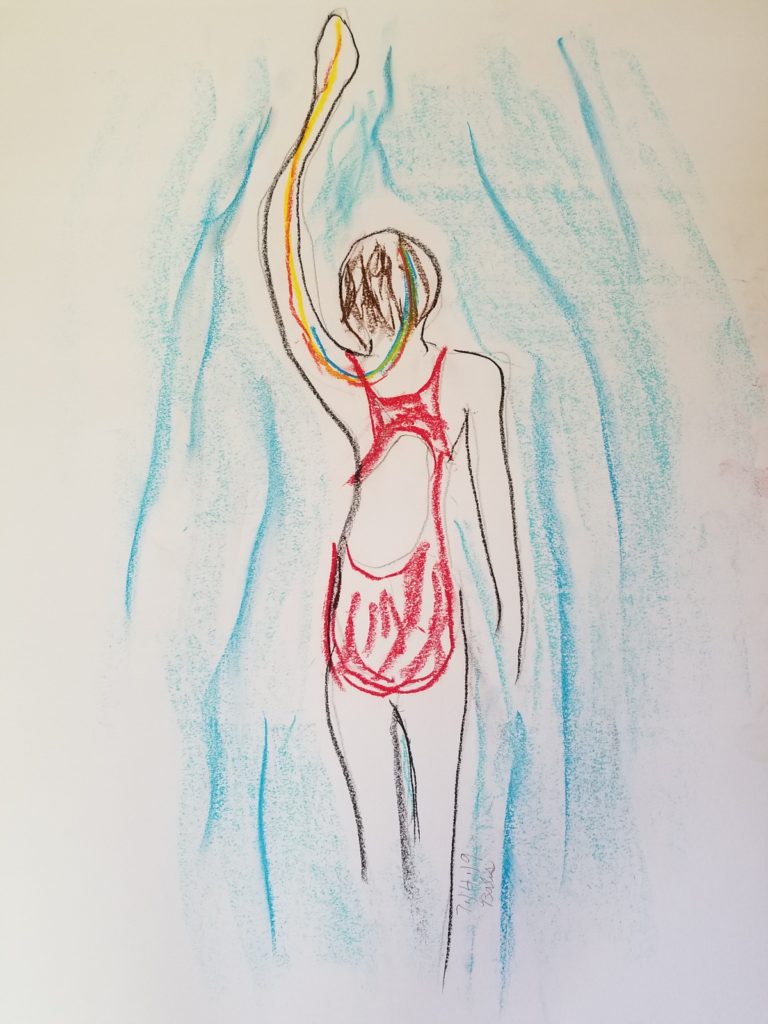 July 2019: Swim, pencil, charcoal, and pastel
July 2019: Swim, pencil, charcoal, and pastel
I love to swim. Before my stroke, I swam three long-distance, open-water swims every year. I have an endless pool at home, so I had logged many hours swimming. Swimming requires strong deltoid muscles, strong shoulders, the ability to straighten your arm and hand, and an even kick.
This APA drawing was meant to stimulate and support the right motor cortex-to-deltoid and right motor cortex-to-hand connections. It’s difficult to say whether it helped me with swimming, given my need to simultaneously strengthen my recently innervated deltoid. To complicate my recovery, in November 2018 I had torn my left rotator cuff trying too hard to swim the crawl (and doing Downward Dog yoga poses) before my body was ready. Waiting until my body is ready to move in more advanced ways was a bitter but important lesson for me. However, every day I am closer to swimming the crawl properly and I believe this drawing reminds my brain that swimming is a goal.
 July 2019: Run, pencil, charcoal, and pastel
July 2019: Run, pencil, charcoal, and pastel
I love to run. Pre-stroke, I ran 3 to 4 times every week. I have completed 6 marathons. The day after my stroke, the Hospitalist told me I would never jog or run again. Why would a medical authority figure limit a patient’s recovery with such a negative pronouncement, especially so early after the stroke? Recall that I had faith in my body to recover and did not understand the severity of my injury. That dire prediction was all I needed to hear to determine that I would one day jog and run again.
I have begun to slowly jog; not too far or for too long, but that will come. Running requires a functioning connection between the motor cortex and the anterior tibialis (purple line) and soleus (orange line) leg muscles. The anterior tibialis is used in the heel-strike phase, and the soleus is used to push off with the toes. In this APA drawing, I added the deltoid connection (red line) for fun.
 July 2019: Magnolia, tempera and colored pencil
July 2019: Magnolia, tempera and colored pencil
Many years ago, I took a photograph of a magnolia bloom in our yard. I always loved that photograph, so I thought I would try another dabbing project. I was not as pleased with the result as I had hoped.
As I dabbed, I kept thinking that this painting would look better with brush strokes. I thought I should have tried using brush strokes since my wrist was extending much better. Additionally, dabbing is a time-consuming technique. I was impatient to continue trying new ways to move my hand and wrist.
 August 2019: Smile, pencil, charcoal, and pastel
August 2019: Smile, pencil, charcoal, and pastel
I consider mouth drop a barometer of my progress. The zygomaticus major muscle enables us to smile. I felt an improvement in my smile after drawing this brain-to-zygomaticus-muscle connection. I could pull my lip up farther than I could previously, and Ken confirmed the improvement. In November 2019, my primary care physician commented that I had no face drop at all! That was not an accurate assessment on her part, but I am getting closer. I feel that when my smile is complete, my full recovery will not be far behind. If you can smile, do it often!
In September and October 2019, I was given the opportunity to hang a show of my artwork in a local restaurant. Having this show gave me a deadline that urged me to continue painting throughout the summer. I was overwhelmed by the support I was shown at the opening reception and throughout the show. I included a short explanation of each image, hoping to educate others about the effects of stroke and the possibility of recovery.
 October 2019: Guzei, pastel
October 2019: Guzei, pastel
Ken and I visited Butchart Gardens, Victoria, British Columbia, in September 2019. I fell in love with the Japanese Garden. Japanese gardens are meant to connect people with nature and to encourage reflection and meditation. One of my other therapies is a daily meditation practice; I enjoyed the Japanese Garden immensely. Since my wrist was extending better and I had found some success with my APA pastel drawings, I thought I would try doing another landscape drawing with pastels. I did this drawing from a photograph I took in the Japanese Garden. A guzei is a red Japanese bridge, and it has spiritual significance as a symbol of transformation.
I found that landscape drawing with pastel, which I had not tried since I drew the Tallassee Oak a year earlier, was frustrating because I still could not draw and fill in small shapes. I felt like I could only move forth and back with the pastel chalk, scratching and scribbling. Round and curvy shapes were still elusive. A comparison of this drawing with the Tallassee Oak drawing will allow you to draw your own conclusions about my improvement over the 12 months between drawings.
 November 2019: Japanese Garden, pastel
November 2019: Japanese Garden, pastel
I was determined to try another pastel drawing. This time, I wanted to concentrate on small, curvy shapes. One thing I did not count on was how readily pastels smear if you rest your hand on the paper, even briefly, while drawing. I needed to rest my hand to draw the small and curvy shapes that I wanted to create.
Although I had just purchased a larger pastel set with more colors, I was also frustrated with my inability to blend colors. In contrast, with tempera I could blend the paint to create any color. I could hold the pastel chalk better than in earlier pastel drawings, but I continued to find proper holding a challenge.
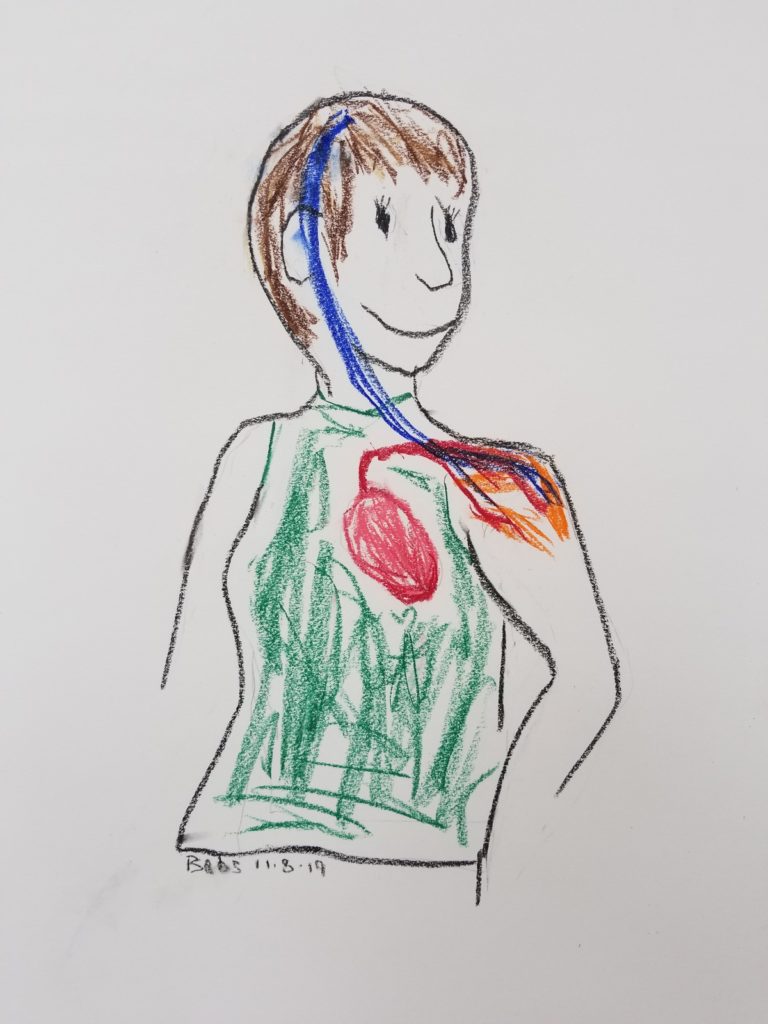 November 2019: Shoulder Connections, pastel
November 2019: Shoulder Connections, pastel
Recall that I was rehabilitating a torn rotator cuff at the same time I was strengthening my deltoid. In November 2018, an orthopedic surgeon had told me that one of my rotator-cuff tears was a “probable full surface tear” that would never heal, but that surgery was out of the question because I would need a functioning deltoid to do the post-surgery rehabilitation. A year later, I was strengthening my deltoid and gently using my rotator-cuff muscles. I cannot be sure of success, but my goals are to fully strengthen my deltoid and to avoid rotator-cuff surgery. With these goals in mind, I decided to expand my APA drawing to include rotator-cuff healing.
This APA drawing is showing my brain (and body) that I want it to enlist my heart in healing by sending blood to my rotator-cuff muscles. I also included the brain-to-deltoid nerve connection, because I figured I cannot overemphasize my deltoid’s innervation. I would need another MRI to know if my rotator cuff is healing; however, I continue to gently use these muscles during my thrice-weekly weight-training workouts.
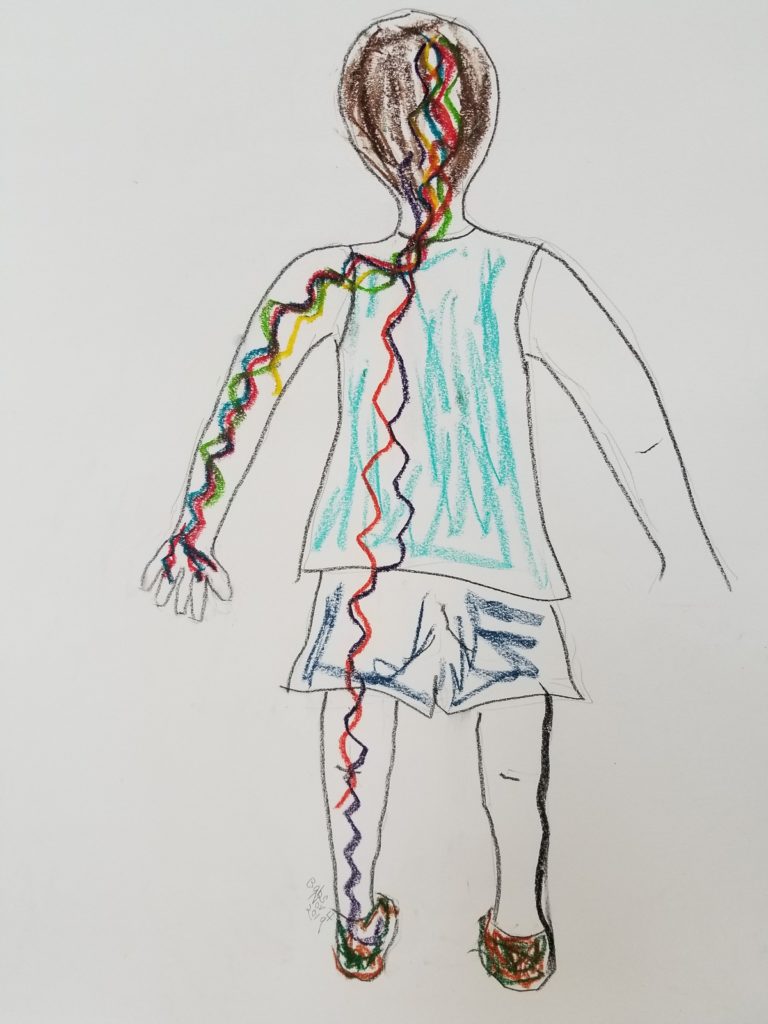 November 2019: Relaxing the Muscles, pastel
November 2019: Relaxing the Muscles, pastel
Despite my continual improvement, I knew that one of my biggest challenges is tone (or spasticity). I needed to find a way to reduce tone in my left bicep, thumb and fingers, calf, soleus, and ankle. Other than Botox and muscle relaxers, no one had any recommendations for reducing tone. I began a self-designed program of targeted stretching and brought out my pastels for another APA drawing to reinforce the message of relaxation. I asked several friends and therapists for advice on how to draw relaxation. A friend who is an accomplished artist suggested wavy lines.
This APA drawing shows my brain that I want my muscles to relax. I was so excited about this drawing I drew myself out of proportion! One of the advantages of drawing and painting with a hand affected by stroke is that your inner art critic is no longer in charge. I did this drawing at the same time I was stretching twice daily, so it is impossible to conclude whether my improvement was a result of one, the other, or both therapies.
 December 2019: Near Machrie Moor, Isle of Arran, Scotland, tempera
December 2019: Near Machrie Moor, Isle of Arran, Scotland, tempera
I wanted to come full-circle to close this essay with another “brush-stroke” painting. Recall that when I dabbed “Magnolia” in July 2019, I thought that the magnolia would be better depicted using brush strokes. The thought of trying another brush-stroke painting stayed with me. I created “Near Machrie Moor” so that you may compare it with my first painting, “Boat in Loch Harray.” Both were done with tempera using brush strokes over just a few days. With this more recent painting you can judge for yourself whether I have made progress with my hand and wrist mobility.
As I painted “Near Machrie Moor,” I felt that I had significantly better control of the brush. Unfortunately, better brush control unleashed my inner art critic, which had previously and thankfully remained in the background. If you look closely, you can see how I painted over and over to correct mistakes. I had to force myself to declare this painting complete.
Art as a Way to Push Limits
I plan to continue my drawing, painting, and photography projects. I feel that these experiences have enriched my recovery experience and have supported my brain’s neuroplastic response. Art has been a creative and rewarding way to push my limits, and it has given me tangible evidence of progress. I am proud of my art accomplishments. Doing art reminds me to take my time and enjoy my success. It has taught me that there are no failures in my recovery, only new challenges.
In this essay, I have shared a selection of my artwork to describe how I have used art as a physical therapy for upper-limb recovery from stroke. I have done all painting and drawing independently, although I would have benefitted from expert guidance in supplies and techniques. When I began drawing and painting, I searched for information on how to heal physically through art. I found many examples of the emotional, spiritual, and social benefits of art therapy. I can attest to these benefits, as I have also experienced them through my post-stroke art projects. I did not, however, find information detailing the employment of drawing and painting to facilitate neuroplastic changes with a direct motor benefit. I feel that this literature must exist, but my searching came up empty.
Autophysioartistry as Rehabilitation Therapy
Given the imperative to foster gross and fine upper-limb movement in stroke survivors, using various art media is an inexpensive and engaging therapy available to everyone. Drawing and painting may foster neuroplasticity as well as, and more creatively than, some of the more traditional occupational and physical therapy techniques. I have only scratched the surface of possibilities. For less mobile stroke survivors, for example, perhaps collage is an option. I have experimented with photo image editing software to facilitate APA drawings by stroke survivors less comfortable with or less able to draw their bodies. I am encouraged by the opportunities made available by photo editing software and hope that others in stroke recovery will use any means available to create art—including APA—to foster their progress.
With its substantive combination of emotional, spiritual, social, and physical benefits, art should be explored, employed, and researched as a physical (and occupational) therapy for stroke survivors and others healing from upper-limb and neurologic injury. I also feel that extending visualization therapy into more concrete visualization including the brain and nervous system using APA (autophysioartistry) deserves the attention of physical and occupational therapists and researchers.
Since my stroke, I have participated in more than 30 different therapies. Many of these are standard therapies and some are novel. Based on the stroke-recovery and stroke-related research I’ve read, I created some of my own therapy techniques. This essay describes one of my self-styled therapies.





 October 2018: Tallassee Oak,
October 2018: Tallassee Oak,  January 2019: Southern Utah,
January 2019: Southern Utah, 





 April 2019: Brain to Hand Connection,
April 2019: Brain to Hand Connection,  May 2019: Woodland Ransome Wildflowers, Lake District, England,
May 2019: Woodland Ransome Wildflowers, Lake District, England,  June 2019: Village Bay, Hirta, St. Kilda, Scotland,
June 2019: Village Bay, Hirta, St. Kilda, Scotland, 

 July 2019: Swim,
July 2019: Swim, 

 August 2019: Smile,
August 2019: Smile,  October 2019: Guzei,
October 2019: Guzei,  November 2019: Japanese Garden,
November 2019: Japanese Garden,  November 2019: Shoulder Connections,
November 2019: Shoulder Connections, 
 December 2019: Near Machrie Moor, Isle of Arran, Scotland,
December 2019: Near Machrie Moor, Isle of Arran, Scotland, 
 Member since 2019 | JM14274
Member since 2019 | JM14274


NO COMMENT