Three Voices at the Table
doi: 10.18737/0607112340
AMA Citation: Riske T, Zorn CR. Three Voices at the Table. J Hum Rehabil. 2018; Fall. doi:10.18737/0607112340
Table of Contents
We gather at tables for different reasons: to eat Thanksgiving dinner, sing Happy Birthday, or play cribbage. Often a place to celebrate milestones, tables are where we create memories with friends and families. At other tables, people come to seek understanding and search for help.
Wayne and his wife CeCelia met Tania, a Speech-Language Pathologist (SLP), at the table in her hospital office. Wayne has primary progressive aphasia (PPA), a rare neurological disease resulting from abnormal brain changes. His ability to speak, write, read, think, and understand others is slowly declining. Eventually, Wayne will have no speech.
Around this table there is less to celebrate. Yet, this team of three has developed relationships, collaborated to construct meaning, and designed strategies to support Wayne’s independence.
In this article, three voices are present. Wayne and CeCelia’s voices will be heard through CeCelia’s description of incidents, feelings, and perspectives, detailing their experience of adapting to Wayne’s challenges over time. Tania, as an SLP, chronicles her interpretations and treatment interventions, grounded in the science and art of speech language pathology.
CeCelia
When Wayne was first diagnosed three years ago, I simply told people, “He has a hard time finding the word he wants to say.” Wayne pointed to his head and then his mouth and said, “I can’t speak.” Neither of us said anything more.
Our minimizing strategy reflected several possibilities. Perhaps it was all we understood or all we thought others wanted to hear. Or perhaps it was all we could bear to say—like dipping our feet into icy water, one toe at a time.
People responded with a nod, an attempt at understanding: “Yup, I know just how that is,” someone said. “I’ll be thinking of something but the exact word won’t come. Just happened today; I couldn’t think of my cousin’s name.” Another said, “Oh geez, nothing to worry about. Happens to my wife and me all the time.” Someone chuckled and said, “Sounds like when my dad had a stroke. All he could do was swear.” People often said, “It’s hell getting old, isn’t it?”
Wayne smiled at all of this.
But I wanted to scream, “This isn’t about forgetting a name. It’s not about getting old or swearing. This is different.”
Tania
When I met Wayne, his language was surely compromised. He struggled to put thoughts into sentences of even 3 to 4 words, grasped for a word for painful stretches of minutes, and had difficulty choosing “yes” or “no.” I didn’t need the pages of doctors’ notes delineating Wayne’s diagnosis to figure it out; we all understood that Wayne’s thoughts and ideas remained as bright, insightful, and humorous as ever, but were being buried more and more deeply by his diminishing language.
Of course, I came into this situation much later than Wayne and CeCelia. They were working hard navigating Wayne’s PPA, learning to communicate with fewer words, relying on routines and shared knowledge, and slowly shifting the balance of their relationship. Wayne’s changing language was stripping away his independence.
I explored the increasing emptiness of Wayne’s language. Key words essential for communicating his intent were lacking. I discovered the phrase, “I did it,” meant an array of activities and experiences, from golfing to building a birdfeeder to going to a concert. When I didn’t immediately grasp what Wayne was saying, I saw the question in his eyes: “Why don’t you understand what I’m telling you?” He often didn’t recognize the vagueness of his language that left family, friends, doctors, and me stumped.
Sometimes I longed to give in to the temptation of pretending I understood; it would certainly be easier. Wayne could save face rather than flounder in word-finding, and I could bask in an illusion of expertise. It was hard work to communicate even then, yet we usually bridged the gap between thoughts and words. Sometimes the journey to common understanding was awkward and ugly. Still, we got there eventually. But that was then.
Note: Primary Progressive Aphasia is not “old age,” Alzheimer’s Disease, or aphasia from a stroke or head injury where language usually plateaus or improves. This is a degenerative disease with a trajectory of decline. There is no going back.
CeCelia
When we met as teens Wayne’s love of music charmed me. Perhaps it was because there was little music in my life. What I heard was limited to an occasional small radio and record player constrained by a short battery life and songs sung by a mournful group shrouded under the roof in the back of the church.
Then I met Wayne. He was singing “Sixteen Candles,” “Love Me Tender,” and “Never My Love.” Singing and whistling and smiling—in the car, in the shower, on a picnic—he knew every word in every song. It was magical and I was riveted.
Since the 1960s, Wayne’s preferences changed but he never lost his skill and love for music. Sometimes it was country, pop, Tina Turner, or Uriah Heep, but the oldies prevailed.
Bette Midler would have smiled hearing Wayne sing “The Rose” at a family wedding. Eight years ago, Wayne sang “How Great Thou Art” at my mother’s funeral—every verse in his rich and fervent voice. Everyone turned to the balcony to see who was filling that same church I attended as a teenager.
Then things plummeted.
A year ago, he could sing only the chorus of the same song at his sister-in-law’s memorial service. With his finger pointing to every word, and support from the choir and organist,
Wayne hobbled through the service but there was little strength and no richness.
Now there is never a hum, never a whistle. Rarely, there is a tentative mumble of a phrase from a song.
Yet Wayne still plays music at home and in the car. At a recent public performance his hands and a foot moved to music. I yearn for those moments to last forever.
Tania
Wayne is one of the most fascinating people I’ve ever known. He’s travelled the world. He eats sushi proficiently with chopsticks, crafts beautiful stained glass artwork, and racks up noteworthy golf scores. He’s cool and cultured, but still outdoorsy and can fix anything. Wayne is a dying breed in today’s world.
I see Wayne’s appreciation for music, his pride when we talk about CeCelia’s flute lessons, and his enthusiastic “I like it” when we talk about concerts. I imagine a rich singing voice that would fill your soul until it nearly bursts, but I’ve never heard Wayne sing. If the future had been more clear, could there have been a chance to capture the last moments when music was still in his voice?
I’ve recorded Wayne speaking brief, rehearsed sentences. It’s a process. I write the sentence and say it, with Wayne watching and listening closely. He practices before we record, imitating my words and intonation, watching me for feedback. When I nod, he knows he’s got it right. After another round of repetition, we record.
The nostalgic, wistful part of me mourns what is lost, and wants to preserve the past, while the clinical side of me strategizes for the future. We no longer pursue language remediation goals, but explore interventions building on Wayne’s strengths: writing, drawing, and coordinating text and audio.
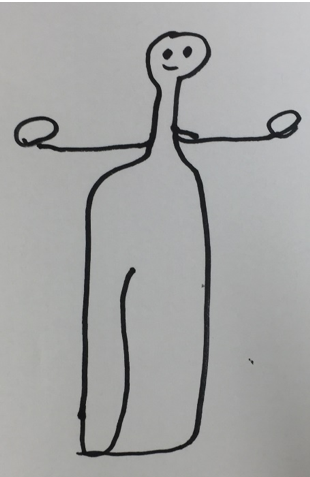
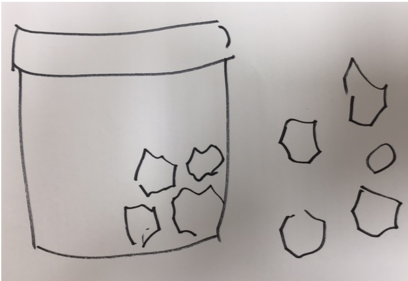
One of Wayne’s many gifts is drawing; he is a master of using it to communicate. (See Figure 1: Bird Girl Sculpture; Figure 2: Birdhouse; and Figure 3: Mosaic-Tiled Project.) The first drawing that Wayne made during a conversation was a stick depiction of himself swinging a golf club, accompanied by a number (76, I think) indicating his golf score that day. In under a minute, he communicated more using that picture than 20 minutes of groping for words and answering my questions.
As our relationship grows, I want to know more about this man, hear his stories, talk about plans for the next adventure or even tomorrow’s mundane activities. Things I can tell you about Wayne: he can’t wait for spring so he can get out and golf, he cherishes time with friends and family, he is a stickler for detail in craftsmanship, and he loves a good scary novel. Like his singing, much of this identity is now buried deep under aphasia—beyond our grasp.
Note: A major therapy goal for individuals with PPA is to support their identity. That is, how do people see themselves and how do they want others to see them? Losing language often results in losing identity and growing socially isolated. Therefore, creating social opportunities and managing social barriers become a key focus of treatment.
CeCelia
Wayne’s go-to words change over time. For several months, to the point of annoyance or embarrassment, he repeated the word “really” in response to almost any comment. Now, dozens of times a day, he goes to, “What’s it called?”, “Well, I don’t know”, or “Like that.” Wayne also had a bout with “Constantly.”
We still laugh about “Constantly.” During a clinic visit, a medical assistant hammered through the usual questions (eg, Do you smoke? Has your weight changed recently? Do you feel safe at home?). Wayne answered each question spot-on.
Then she asked, “Do you drink?” and, you guessed it, Wayne smiled and said, “Constantly.”
The medical assistant never blinked, looked away from the computer screen, or asked any clarifying questions. I choked down a giggle, knowing Wayne meant his one or two drinks at every day’s happy hour. I haven’t a clue what she recorded. Is there a space to check “Constantly”?
Wayne’s failing ability to think, plan, and problem-solve extends far beyond repetitive words or phrases. Like all other things with PPA, there is no recovery, no return.
Wayne never met a place he couldn’t find. He was a coach driver taking tour groups to nearly all 50 states before GPS existed. Pages he printed from MapQuest hung by his steering wheel—from Los Angeles to Boston, Miami to Anchorage. He made it look so easy. Now, although the GPS helps, he is not able to negotiate unfamiliar places and their road signs.
This may seem trivial but Wayne focuses on only one thing at a time and seeks affirmation after every task. For example, when Wayne cuts celery while we’re cooking, he asks repetitively, “Is this OK?” My patience used to fade after the first few times but now it’s easier for me to look and say, “It’s perfect,” especially if it’s in the ballpark. If I don’t look, it’s not OK.
Wayne needs repeated directions.
“Yes, put the celery in that kettle.”
“In here?”
“Yes, in that kettle.”
“Put it in here?”
“Yes, in there.”
“Like this?”
“Just like that.”
Because of Wayne’s lack of speech and thinking skills he’s unable to make or take phone calls. There’s an occasional FaceTime with his brother, although some of these connections went better than others and their frequency has dwindled.
Wayne is skilled at smiling, nodding, and saying “yes” so people believe he understands. But I sense he often doesn’t understand. His cognitive loss is the hardest to describe—hardest because it hits me with a bigger hammer, a more crushing blow.
Tania
Over the past year, I’ve witnessed Wayne’s language change from hard-won short sentences to a smattering of single words and automatic phrases. The energy we spend to establish a common reference (I think of it as “getting to the same ZIP Code”) can be exhausting. While Wayne is skilled at drawing, gesturing, and using apps on his iPad to communicate, it is still a formidable task to introduce a topic and often becomes a guessing game.
I know a handful of tricks to get us to a common understanding, but Wayne’s aphasia limits his contribution to conversation. He rarely expands upon the most basic information, offers commentary or opinion, or asks questions. Like an interviewer, I probe with questions and comments to prompt Wayne to elaborate. While this strategy expands the conversation, inevitably I become the controller, navigating the twists and turns of the exchange. The conversation is no longer Wayne’s, nor is it a collaborative experience. Instead, I become the director of Wayne’s expressions.
Wayne’s eyes express relief when I direct the conversation. It’s easier for him to select a choice from a field of written options than to formulate his own thoughts and words. Aphasia has turned the freedom of initiating topics, asking questions, and sharing unique thoughts into a prison of words. When I write a list of choices for Wayne, the prison door inches open and he points to the word that reflects his intent. But it’s really only a shallow scratching of the surface. While Wayne can select one of my written words to tell me he went skiing over the weekend, there are no written choices to describe the fresh snow, the smooth glide of the skis, and the escape from words. When I run out of questions, the conversation dies.
Note: Strategies to help individuals with PPA communicate are (a) patient-initiated, or (b) partner-supported. In his face-to-face or e-mail communication, Wayne uses the whiteboard, dictation, text-to-speech, and map features on his iPad. He’s comfortable with the technical use of these features, but his communication is often limited by his struggle to dictate a word or phrase. Partner support is essential in most cases, particularly with provision of written scaffolding (eg, a list of words, yes/no, 1 – 10 scale of like or dislike). This works if there is a convenient pencil and paper or iPad. But this is not convenient or socially natural in many situations, such as while driving a car, listening to a concert, sitting around a living room, taking a walk, biking, or skiing.
CeCelia
Wayne enjoyed reading a variety of fiction and nonfiction. Stephen King was a favorite. When we book-shopped, he pulled out his yellow, creased paper listing nearly all of King’s 50-plus novels and many short story collections. Wayne bought the first clunky Kindle and wouldn’t leave home without it.
But like his speech, Wayne’s reading is also slithering away.
Last week, Tania asked Wayne about the next audio book he’d be reading. He had just finished listening to Spare Parts in a three-week aphasia group activity. Wayne looked at Tania blankly and said, “Well, I don’t know.” Tania and I glanced at each other knowingly; selecting and downloading the next book never crossed his mind.
That evening, after kissing good night, I asked Wayne again about his next book. His “Well, I don’t know” response told me, enough is enough. I must learn—stop pushing, things are different now, so live with it. Yet, I keep urging.
Wayne’s diminishing reading and writing skills pummeled me when I saw my name misspelled and crossed out several times in the Valentine’s Day card he gave me. Now he writes my name from a copy and picks out cards based on the picture. This is a guy who drilled me with every card he gave me over the past 40 plus years, “Are you sure you read it?” I have to admit, sometimes I just skimmed the Hallmark verse.
Reading and thinking have become heavily, sometimes exhaustedly, collaborative activities. Ordering from a menu and completing a credit card transaction can no longer be done independently. On his birthday last year, Wayne received a couple of cards. Some family members probably have no idea he has little reading ability and that I needed to read them for him. I wonder what they would send if they knew.
Although Wayne can draw a picture or write a word (misspellings aside), most other writing is lost, especially writing required on-the-spot. Clerks write out checks for him at businesses that don’t accept credit cards. We’ve received no Red Alerts from our bank. So far so good, although our online banking has hit a few not-too-serious bumps.
Though it takes 20 to 30 minutes for us to compose a one-or-two-sentence e-mail message, the outcome is usually muddled. I try not to correct every error or dictate the message (although that’s becoming increasingly necessary). I hope the recipient understands and forgives the sender.
I’m practicing patience at a level that challenges me daily. I don’t always succeed. Further, I’m always torn between just doing or saying things for him, versus waiting, encouraging, and honoring Wayne’s fading independence.
Tania
Verifying information with Wayne is essential. When he creates a drawing, I double-check to confirm my interpretation is correct. I’m usually on the right track; Wayne’s a capable artist and his drawings have enough detail. But verifying is difficult. Wayne oftentimes says “yes” when he means “no”, and vice-versa. To complicate the issue, aphasia limits his recognition when this happens, and opportunities for misunderstanding abound.
When Wayne uses text-to-speech to accompany his reading, he is excellent at identifying facts in news stories. I ask him to focus on the headline and first sentences to identify and share a main concept. He’s pretty good at that, often stating an idea that mirrors a headline word-for-word. But few good conversations are made by simply sharing a headline. When I ask Wayne, “what do you think about that?”, his response is predictable, defaulting to one of his automatic sentences, “Well, I don’t know.”
When I press Wayne, he combs the text for something to satisfy my request. Often he repeats what he’s already shared. Other times, he unearths a minute detail buried in the text, copying it with little comprehension. My list of written choices gives Wayne the opportunity to select his preferred weekend activity, or he points to a spot on a rating scale to indicate how much he enjoyed a play he and CeCelia attended. But I have yet to find a reliable strategy for Wayne to initiate a novel turn in topic, pose a question, or ponder a point of interest. Wayne has done each of these things, but only once or twice, with painstaking effort and a level of support that hovers near the therapeutic reporting term “maximum assistance”.
I know it is unlikely that Wayne will carry these conversation burdens alone. Conversation is an art of balance, give-and-take, sharing of a load—but aphasia tips the scale. Aphasia has stolen his independence to hold his end of the exchange. His interactions are increasingly limited to the creativity and inquisitiveness of his partners.
Note: With PPA, roles change in obvious ways. One question emerges: Does the spouse, partner, or family live with an individual who has PPA? Or does the spouse, partner, or family live with the PPA that invaded the individual? Perhaps it alternates—sometimes one, then the other.

CeCelia
As the months went on, Wayne visibly struggled when he tried to say a word or express something he wanted to share. In these situations, other people’s discomfort often intensified. Some looked down. Others turned toward the door or the window when Wayne tried to think of a word. Others checked their phone.
When Wayne showed a physician his aphasia card describing his abilities and helpful communication strategies, the physician said with a swagger, “I know all about that—from before.” He didn’t look at Wayne’s card.
“It’s different now,” I said, glaring with my voice on the edge of crackle.
“Really? So how’s it different?” I thought I heard skepticism in the physician’s voice, but maybe I imagined it.
“It’s getting worse,” I said, more brusquely than I intended. It was only after I explained that Wayne’s aphasia was progressing that the physician backed off and apologized.
As Wayne’s aphasia progresses, people’s reactions vary. At a dinner at our home, while Wayne was fighting to find the words, one person actually got up from the table to use the bathroom. Frequently, two people will begin a side conversation. Some previously close family members have distanced themselves. Others ask, “You’re in therapy. Is it getting better?”
I’m not sure how to interpret any of these reactions. Are they uncomfortable with Wayne’s aphasia, not understanding, or not knowing what to say or do? Am I jumping to conclusions?
In the end, maybe it doesn’t matter what people think and know. Although I’m convinced people’s reactions are not intentionally hurtful, I don’t want Wayne to see others’ lack of understanding or clumsiness. He feels sad about his losses; he doesn’t need to see or hear when others are struggling. I often run interference, dismissing what we’re witnessing.
I don’t want Wayne to notice anything is different. But I know he does.
A revered, family old-timer who adores my husband recently told him, “Why the hell did this happen to you? I wish it would’ve been me instead of you.”
Wayne smiled; I think he felt the shared love. If I would ask Wayne about the old-timer’s comment, I suspect he would say, “I like it.”
If Wayne likes it, I like it too. That is my life-saver ring, my life preserver, for now and for always.
Tania
That day at the grocery store was just luck. I was making a mid-week stop to grab fridge staples when I saw Wayne standing next to a wide-eyed store employee, pointing to his iPad. I saw the shape of Wayne’s words, “What’s it called?” Seeing the employee’s eyes darting around seeking an escape, I walked up and said, “Hey.” The employee uttered a relieved “Thank you” and vanished. Glancing at Wayne’s iPad, I saw what he had been pointing to: the words “small can of chopped green chiles.” He needed to find the chiles.
Most of us take for granted the ease with which we can seek help for everyday tasks. At the store that day, the words Wayne needed to ask for help were lost between aphasia and a well-intentioned, but uneasy employee. Would he have located the chiles eventually? Maybe. Or maybe he would have given up and walked out. Either way, this was a sucker punch reminder that the strategies we practice to supplement Wayne’s language are not fail-safe outside of the security of the therapy room walls.
It’s not a lack of motivation or disinterest in others that underlies Wayne’s passiveness in conversation. I know Wayne recognizes the loss and changes in his interactions. But in my opinion, he doesn’t focus on that. Instead, he turns to me to help him learn tools that assist him now. He often tells me, “I like it” when we stumble upon a new strategy or have a moment when communication flows smoothly. I have never heard, “I hate this,” or “This really sucks.” I suspect it’s not due to lack of words to express this sentiment, but rather Wayne’s choice to “like” the lot he’s been handed. He comes to therapy unfailingly, puts every ounce of energy into difficult tasks without a flicker of annoyance, and diligently completes his homework.
I think about CeCelia often, and how her life has changed as Wayne’s aphasia progresses. She chastises herself for not being more patient, yet I’ve never seen a partner more patient, positive, and discreetly supportive. Instead of jumping to conclusions or taking over the conversation, CeCelia has an uncanny knack for making an inclusive comment that subtly fills the gap for Wayne. It’s like a code between them. It’s no secret Wayne relies heavily on her to maintain his independence and social participation, and CeCelia fills this gap gracefully. Whatever she’s feeling inside, I see a partner who makes Wayne’s world complete.
Note: We rely on language to reveal understanding and competence. It’s increasingly difficult to assess these in Wayne, as his language becomes less dependable. We’ve discussed future planning – how to know when it’s time for Wayne to turn over managing household finances and increase collaboration to pay the bills and complete paperwork. More complex issues will need to be addressed in the future—driving, cooking, self-care, and the need for 24/7 supervision.
But for now, our collaborative energies around our table focus on giving Wayne a voice. It’s not Wayne’s old voice; aphasia continues to chink away relentlessly at his power to express his thoughts, ideas, wishes, and dreams. We can’t recover what is lost, but we can cherish his identity and determination to “like it.”
Acknowledgements
We are grateful for others’ suggestions and to the reviewers of this essay: Katherine Schneider, Emily Kinzel, Tom Sather, Mary Beth Clark, Amy Hilbert, Adie Minor, Allyson Loomis, Karen Witt, and Carol Riske. We treasured their help as we planned, wrote, and revised to get things sharp, whole, and careful.
We are most grateful to Wayne for granting his permission to write this essay. Our hope is that his gracious generosity helps others.
About the Author(s)

Tania Riske, MS/CCC-SLP
Tania Riske, MS/CCC-SLP, is a Speech-Language Pathologist at Mayo Clinic Health System in Eau Claire, WI. She treats acute care hospital inpatients as well as outpatients, with focus on development and implementation of functional goals to improve patient and caregiver quality of life. Her therapy approach and values are based on the principles of the Life Participation Approach to Aphasia, with attention to revealing competence and increasing social participation. She greatly appreciates the shared experiences and collaboration with patients and their families, and the opportunity to be a part of the care and support network.

CeCelia R. Zorn, PhD, RN
CeCelia R. Zorn, PhD, RN, is a Professor Emerita from the University of Wisconsin-Eau Claire. In her teaching and research, she integrated humanities into nursing and authored more than 30 articles in peer-reviewed journals, several book chapters, and three books: Becoming a Nurse Educator: Dialogue for an Engaging Career, Angels Don’t Get Tattoos, and Devils Don’t Wear Velvet. Her husband, Wayne, was diagnosed with Primary Progressive Aphasia four years ago. Now CeCelia is continually learning supportive communication strategies, confronting the challenges of a changing relationship, and facing a descending progression. She finds meaning in the following: Life isn’t about waiting for the storm to pass—it’s learning to dance in the rain.
![]()
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.

