A Letter to My Mother
doi: 10.18737/0607783590
AMA Citation: Otiwu EJ. A Letter to My Mother. J Hum Rehabil. 2020; Fall. doi:10.18737/0607783590
Table of Contents
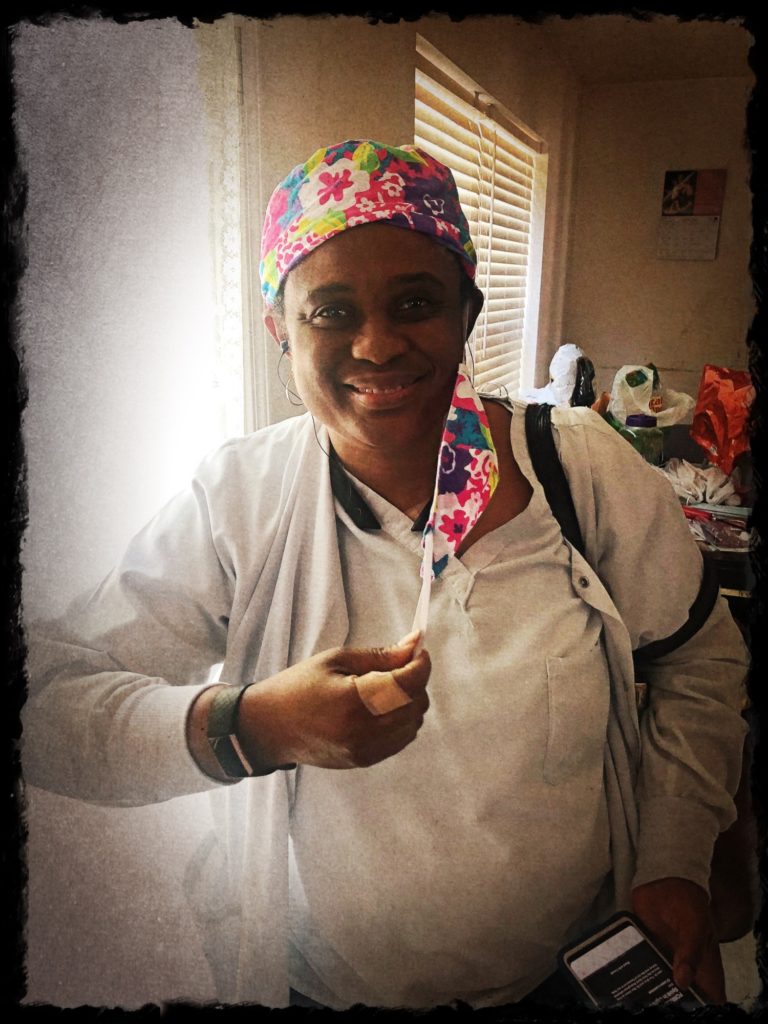
Dear Charge Nurse Mommy,
It is currently 10:47am on June 2, 2020. You have just returned home from another night shift. As a registered nurse, you have been fighting on the front lines against COVID-19 since the pandemic began. However, each morning you return with a smile on your face. In a time where the virus has impacted minorities and people of color more than any other group, you have been forced to face this fact while caring for a disabled family member, as well as four Black boys during this tumultuous time in America. Though your shift ends each morning, your level of stress does not end. Unfairly, it must transfer from one medium to another. Every fear and obstacle that our family encounters each day must be put on hold the moment you leave the house to serve our community.
These notions have become more apparent to me after taking a course on humanism in this second year of my physical therapy studies. This course prodded me to think more deeply about healthcare, reflecting on how those around me who work in, and are recipients of, healthcare are being affected. Through this online course, we have learned that humanism and empathy are, and should be, the backbone of healthcare. Having compassion and understanding for those we treat is unquestionably a basic requirement in our respective fields of nursing and physical therapy.
However, you have told me that with the current required adaptations in healthcare due to COVID-19, patient interaction has been discouraged and limited due to the risk of spreading the virus to others. Nurses are isolated, caring for fewer patients than usual, while abiding by tedious, albeit necessary, time restrictions in each room. The days of conversing with patients and putting them at ease is a thing of the past, as changing I.V.’s and refilling medications are to be done as quickly as possible with minimal social interaction. Worse yet, you are also no longer able to decompress with your nursing-staff colleagues between patients. Nurses are urged to maintain social distancing from one another on the floor, causing you to oversee your small group of COVID-19 patients from a distance, with only text or phone-call communication at your disposal during your “down time.” In addition, longer work hours and increased stress have been imposed upon most urban hospital workers during this time, as these same minority-rich areas have been impacted at disproportionate rates. In these areas, healthcare workers are holding on by a thread, as the threat of burning out in this professional population will certainly rise. Over the past five years, “spending too many hours at work” has been repeatedly voted as a top-three factor in causes of burnout among healthcare professionals.1
Just as it seemed that the odds stacked against our brave essential workers might reach a breaking point, you and other Black healthcare workers were forced to endure additional emotional strains in reference to the various injustices that have now become unequivocally transparent over the last few months. Considering this, the effects of burnout are not only physical; burnout has an emotional toll as well. Research conducted by Thomas Reith demonstrated that in the current healthcare system, over half of all physicians experience some form of burnout symptoms, while 43% of nurses experience emotional exhaustion. This, in turn, can impact their level of care, empathy, and attentiveness toward patients.2 These numbers have been reported at even higher rates in those that are on the front lines of care in emergency rooms and family medicine clinics.1
I fear it is only a matter of time before these numbers soar throughout healthcare and essential personnel as the pandemic will certainly expedite the process. Some have already begun to feel these effects. How will we as a system bounce back once this is over? How will we advocate for much needed change to help the system’s valiant fighters? How will we work to change the country? Though some of the answers may be elusive, one thing is certain: the woman pictured above will walk through those same hospital doors at 7pm, wearing a smile under her mask to serve her patients no matter what may await her outside those hospital walls.
All essential workers are heroes, but Momma, you are my hero. I will keep doing my part to make sure you feel appreciated at home by cleaning and cooking and whatever else is needed. I will try my best to stay safe as well, though I know you will never stop worrying. As a society, it is our time to uplift our healthcare workers and care for them as they have cared for us over the years: with compassion and unwavering determination. We must return the favor and provide a crutch of support realizing that they are mothers, fathers, sisters, and brothers who will need our aid in the post-pandemic world to come.
Love you forever,
Eze
Homepage thumbnail photo by Ezeoyibo Justin Otiwu
References
- Reith TP. Burnout in United States healthcare professionals: a narrative review. Cureus. 2018;10(12):e3681. doi10.7759/cureus.3681
- Joint Commission, Division of Healthcare Improvement. Developing resilience to combat nurse burnout. Quick Safety. July, 2019. Available at: jointcommission.org/-/media/tjc/newsletters/quick_safety_nurse_resilience_final_7_19_19pdf. Accessed: August 17, 2020.
About the Author(s)

Ezeoyibo Justin Otiwu, SPT
Ezeoyibo Justin Otiwu is a third-year Doctor of Physical Therapy student at Emory University. He began his education with a Bachelor of Science degree from Georgia State University. As a first-generation Nigerian-American and first-time author of a published work, he strives to continue learning and using his knowledge of the humanities to impact his professional career by utilizing aspects of compassion, understanding, and cultural awareness to sharpen his clinical practice techniques and decision making. He anticipates a greater use of these learned techniques upon graduation and looks forward to spreading awareness while providing proper patient care along the way.
![]()
This work is licensed under a Creative Commons Attribution 4.0 International License.

