Eye Spy 2022: Improving Nonverbal Communication and Interprofessional Perceptions in Health Science Students
doi: 10.18737/0607224415
AMA Citation: Dodds C, Mulrenin B, Kerr L, Cormack C, Kascak K, Hiester R. Eye Spy 2022: Improving Nonverbal Communication and Interprofessional Perceptions in Health Science Students. J Hum Rehabil. 2022; Spring. doi:10.18737/0607224415
Table of Contents
Purpose: With the theoretical and conceptual underpinnings of Bloom’s Taxonomy and TeamSTEPPS®, the purpose of this study was to examine changes in communication skills and interprofessional perceptions of health science students following visual thinking strategy (VTS) instruction in a museum setting.
Methods: Using a pre- and post-test design, 25 interprofessional health science students at the Medical University of South Carolina (MUSC) enrolled in the 8-week Eye Spy program, developed and implemented in 2018-19 by MUSC faculty and the Gibbes Museum of Art museum educators. The Nonverbal Checklist (NVC) and Readiness of Interprofessional Learning Scale (RIPLS) assessed communication and attitudes related to interprofessional education.
Results: Significant improvements were demonstrated in NVC scores as assessed by students and museum educators. The Professional Identity subscale scores of the RIPLS also significantly improved.
Discussion: Among interprofessional health science students, affective domain development and interprofessional perspective were positively impacted by participation in a VTS-grounded course. Although there is limited evidence, an expectation exists that students displaying higher levels of affective development will be more compassionate and patient- and family-integrated care providers. Future studies should not only explore educational outcomes and strategies within higher levels of the affective domain, but also examine the long-term impact of these affective instructional approaches on actual clinical practice.
In 2018, Eye Spy began as a pilot educational opportunity for physical therapy students to enhance communication and observation skills. With funding from the South Carolina Clinical and Translational Research Institution Team Science Program NIH/NCATS Grant Number UL1TR001450 and Interdisciplinary Research Training in Otolanyngology and Communication Sciences T32 DC014435, this work has now expanded into the interprofessional education arena. Our initial Eye Spy findings and publication provide descriptive and qualitative findings that well informed our current and more objective quantitative work. This current publication offers objective evidence that museum-based instruction can improve the interprofessional readiness and communication of students studying within a variety of health science disciplines.[/vc_column_text][vc_column_text]
Introduction
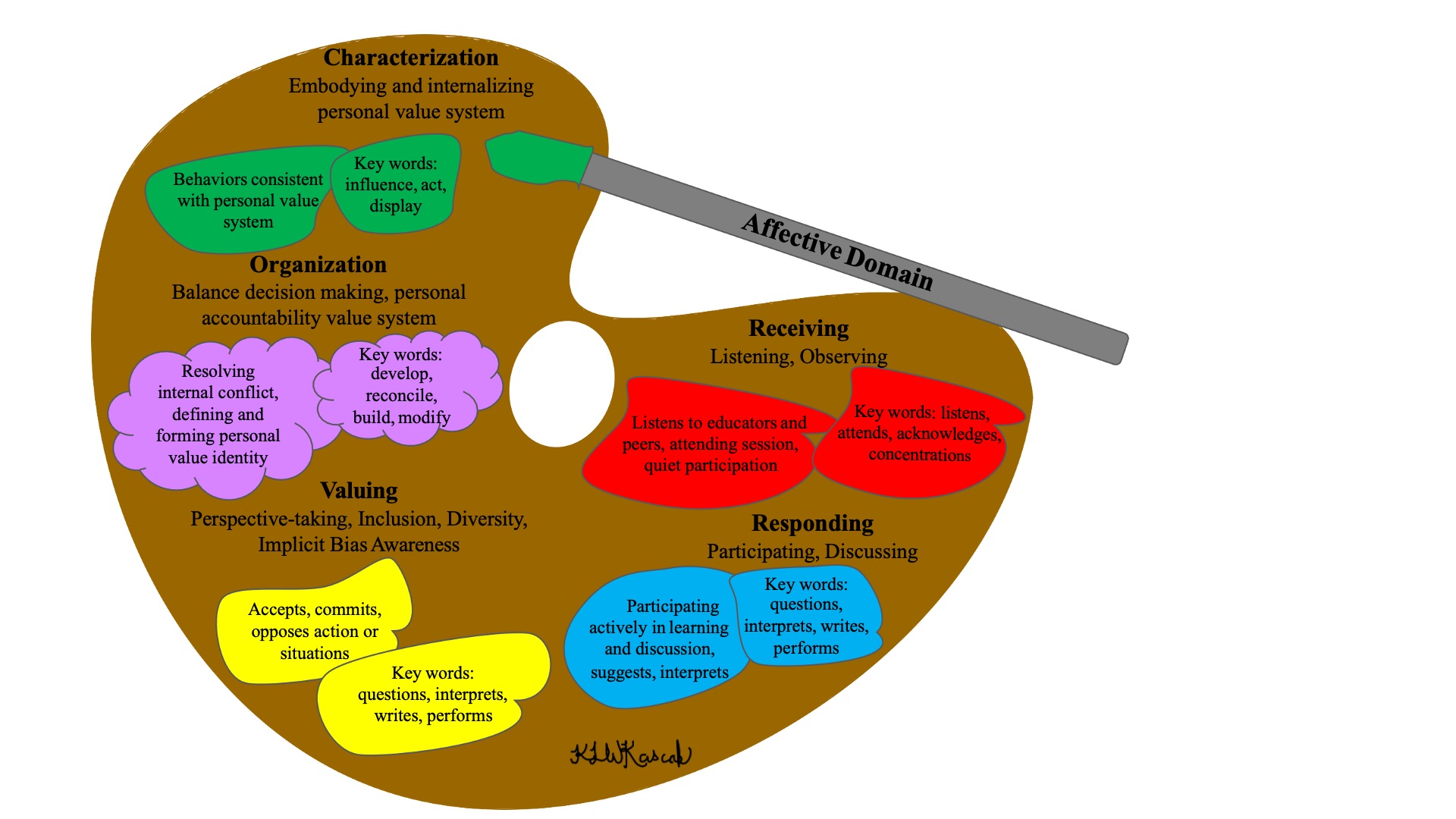
To become competent practitioners, health science students must attain expert clinical knowledge and skills; however, it is equally important for them to develop into reflective and compassionate practitioners.1 Although faculty recognize the importance of affective skill development in health science students, many feel affective objectives are subjective and personal in nature, making instruction and measurement problematic. As such, identifying educational and complementary assessment methods to support and enrich affective development is needed.2 Bloom’s Taxonomy provides a well-recognized framework used by educators for fostering instruction and outlining assessment of educational objectives.3 Commonly overlooked in education are Bloom’s affective categories,4,5 which include receiving (eg, listening, observing); responding (eg, participating, discussing); valuing (eg, inclusion, diversity, implicit behavior); organization (eg, balanced decision making, responsible for one’s behavior); and characterization (eg, value-guide behavior, self-reliance, cooperation, empathy). See Figure.5
The health humanities provide health science faculty opportunities to teach skills linked to Bloom’s affective domains, from the lower levels of receiving and responding to the higher levels of valuing, organization, and characterization. While assessment of health humanities educational initiatives remains problematic to some degree,6 humanities educators argue that engagement with the health humanities can foster observation and communication skills (receiving and responding) while also promoting reflection, perspective-taking, integration, awareness of nuance, and tolerance for ambiguity7—qualities associated with the higher levels of Bloom’s affective domain (valuing, organization, characterization). Narrative medicine practitioners, for example, promote the 3 domains of attention, representation, and affiliation,8,9 with the latter two corresponding to Bloom’s higher levels because they promote not only the understanding of perspectives and values (self and others), but the integration of those value systems and co-construction of meaning. Like narrative medicine, visual thinking strategies (VTS) have come to the forefront of the health humanities as a pedagogical approach that provides students opportunities to observe, listen, think, and construct understanding as outlined across Bloom’s affective domain.10-13
Museums provide a rich environment for embedding humanities into health science education. Compared to traditional healthcare settings and learning environments, museums and their associated art-based experiences are often perceived as less authoritative and threatening.14 As such, observations and communications occurring in museums and/or during art-based experiences allow for a variety of in-depth and diverse interpretations and perspectives. Commonly used within museum settings by qualified museum educators to encourage sharing and discussion, VTS are based on three questions: 1) What is going on in this piece? 2) What do you see that makes you say that? and 3) What more can we find?10
Practicing VTS in museum settings with faculty and museum educators provides health science students the opportunity to safely explore and collaboratively contemplate more poignant inquiries, such as racial discrimination and mental illness. VTS have been successfully implemented in health science education by several investigators. Gowda and colleagues15 created the Observation and Uncertainty in Art and Medicine course to strengthen communication and explore ambiguity in 44 first-year medical students. Surveying students at the end of the course using 3 measurement scales, they noted improvements in students’ awareness of personal bias (Best Intentions Questionnaire), ambiguity (Tolerance for Ambiguity Scale), and reflective ability (Groningen Reflection Ability Scale). They found that only reflective ability increased significantly.15 Katz and Khoshbin16 reported gains in diagnostic skills following participation in VTS for medical students. In other studies, the practice of VTS has been shown to improve clinical observation skills in nursing students17 as well as communication skills and attitudes in nursing and medical students.7
The majority of VTS instructional findings have focused on discipline-specific student populations; however, authors Katz and Khoshbin16 documented VTS work within the Brigham’s Integrated Teaching Unit entitled “Multidisciplinary Teambuilding Museum Workshops.” Following workshop participation, clinical teaching teams suggested VTS could have a positive impact on team building; thus, this provided some of the preliminary evidence supporting VTS’ use within interprofessional practice and education. Beyond measuring the affective impact of VTS on students, our study was also interested in how students’ affective development intersected with or enhanced interprofessional learning. From a theoretical perspective, substantial crossover may exist between the affective domain of Bloom’s Taxonomy and the Team Strategies and Tools to Enhance Performance and Patient Safety (TeamSTEPPS®) framework.18
An Intersection of Components and Principles for Assessment
Developed by the Institute of Medicine and described in the To Err is Human report,19 the TeamSTEPPS® framework was designed to optimize team performance across the health care delivery system. Five key principles are highlighted in TeamSTEPPS®: team structure, leadership, communication, situation monitoring, and mutual support.18 The intersection of these key principles with the components of Bloom’s affective domain is evident.
For instance, Bloom’s affective receiving overlaps with the key principle of situation monitoring, which promotes observational environmental scanning in order to assess and gain understanding of a situation. For Bloom’s affective components of responding and valuing, the key principle of communication is essential, which in TeamSTEPPS® allows clear and decisive exchanges among team members. Bloom’s affective principle of valuing, with its acceptance, commitment, and opposition to action, is central to team structure, because without respect for team structure, effective, efficient, and cohesive teams could not exist. The personal value systems developed within Bloom’s affective organization and characterization provide the foundation for TeamSTEPPS®’ leadership and mutual support. Both Bloom’s affective domain frameworks and TeamSTEPPS® provide structured, teachable opportunities to foster affective and interprofessional learning. To this point, this study used VTS in a museum setting to affect observations, communication skills, and interprofessional attitudes and perceptions of 25 interprofessional students.
While communication is a component found within both Bloom’s affective domain and TeamSTEPPS®, communication itself is made up of three channels: verbal, vocal, and kinetic. The verbal channel conveys the cognitive message, which is delivered by the vocal channel through pitch and inflection of the voice. One support system on which the verbal, vocal message is conveyed is the kinetic channel that includes gestures, postures, and movements. Kinetic, or nonverbal, communication that supports the receiving and responding of communication includes being present (eg, rather than hidden behind computers and smartphones), establishing eye contact, displaying neutral to pleasant facial expressions, angling body position openly toward the individual, and using affirming gestures such as head nodding. Without an appropriate kinetic channel support system, messages conveyed may be misconstrued.
For instance, how might a healthcare provider gathering a patient history with little eye contact, arms and legs crossed, and inattentiveness, most likely be perceived by the patient and family? He/she would probably be seen as uninterested and unconcerned about the patient’s health and welfare, whereas the same healthcare provider with arms open, a forward-leaning posture, maintenance of eye contact, and affirmative nodding would be identified as concerned and caring. Kinetic or nonverbal communication, the silent messenger, can have a great impact on overall communication. These nonverbal communication skills are believed to be important to the development of rapport between health care professionals and patients20 as well as interprofessional colleagues. Training health science students in communication—including nonverbal awareness—is therefore truly important.
The Mixed-Model Eye Spy Study
With the theoretical and conceptual underpinnings of Bloom’s Taxonomy and TeamSTEPPS in mind, we conducted a mixed-model study to examine changes in observation and communication skills and interprofessional perceptions following VTS instruction in a museum setting. The purpose of this article is to present our quantitative findings related to nonverbal behaviors and interprofessional learning. We hypothesized that interprofessional students participating in eight VTS sessions in a museum setting would display improved nonverbal communication skills and enhanced perceptions of interprofessional practice.
Course Development. The interprofessional Eye Spy course was developed and implemented by a physical therapy faculty member within the Medical University of South Carolina’s (MUSC) College of Health Professions and four museum educators at the Gibbes Museum of Art in Charleston, South Carolina. Additional faculty members from MUSC’s College of Medicine, Nursing, and Center for Academic Excellence participated in interprofessional course consultation, development, and implementation. Faculty members reviewed course objectives and outcomes, outlined specific course activities over 8 sessions, and identified collections and locations to be used during VTS instructional activities. The decision to conduct the Eye Spy course over 8 sessions in a 15-week semester was based on evidence from Naghshineh and colleagues,21 who documented greater improvement in the observational skills of medical students following 8 or more art observation sessions. That study’s observational data was qualitative in nature. Our qualitative findings from the Eye Spy course, related to vocal language richness as well as humanistic qualities in observations and written communication, will be reported in a separate manuscript.
Timeline. Seven Eye Spy sessions occurred using art collections at the Gibbes Museum of Art; one session involved collections within the MUSC’s Ashley River Towers Hospital. Up to 10 graduate health science students could enroll each semester over a total of 3 semesters and were allowed to only participate in one semester. Students were recruited into this elective through the MUSC’s Office of Interprofessional Initiatives.
Methods
Design
The study was considered a program evaluation project related to graduate education; therefore, it did not require formal Institutional Review Board approval. However, we obtained students’ consent to participate in the study and be photographed and videotaped. These permissions allowed images to be used for the purpose of describing and disseminating the Eye Spy program to stakeholders at a local and national level.
Participants
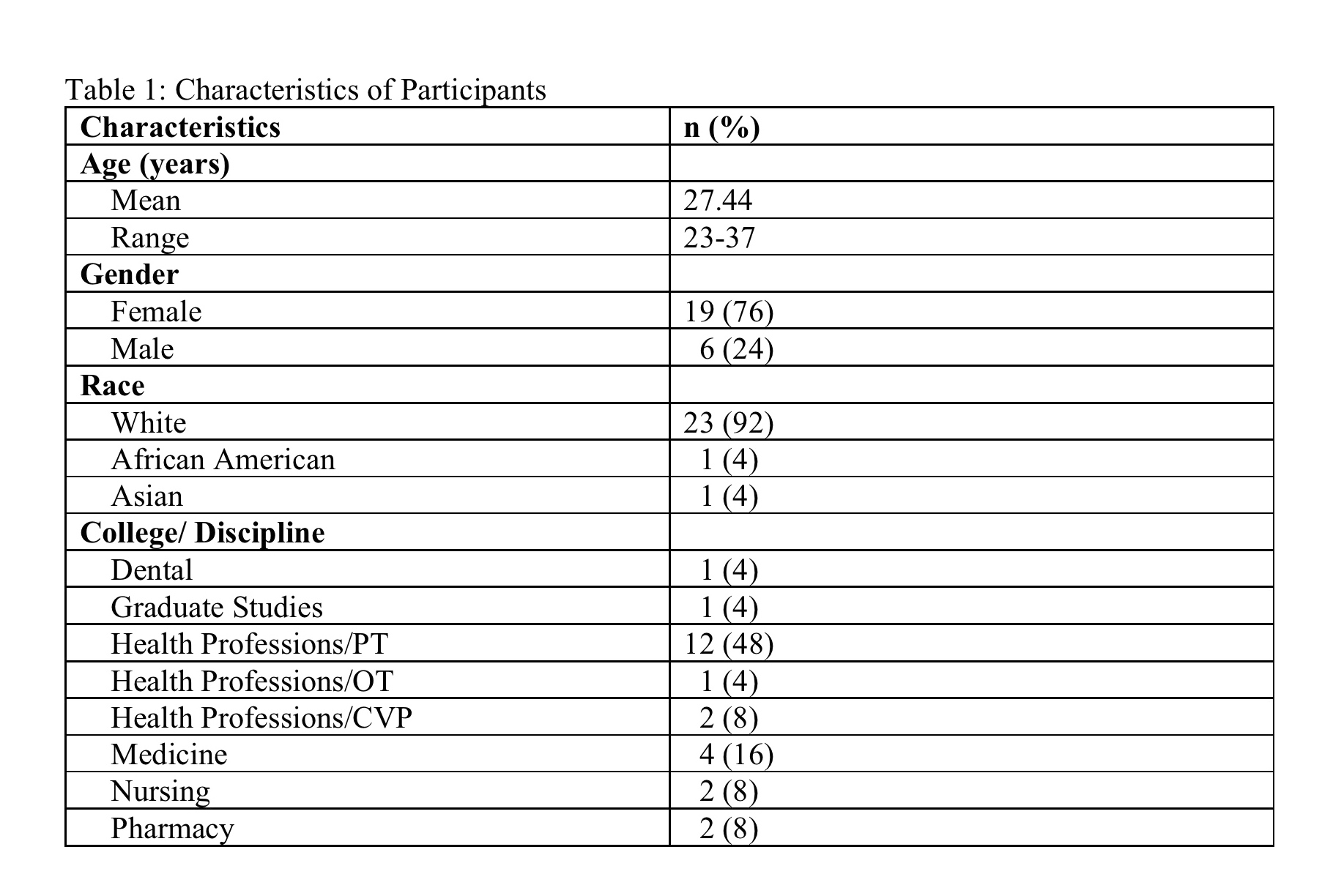
Twenty-five interprofessional graduate health science students participated in the Eye Spy Program. Twenty-four of these students self-selected to take part in the Eye Spy elective. The 25th student enrolled as part of a faculty-developed remediation plan related to continual unprofessional behavior incidents related to inappropriate communication with peers. Table 1 provides demographic participant information.
Outcome Measures
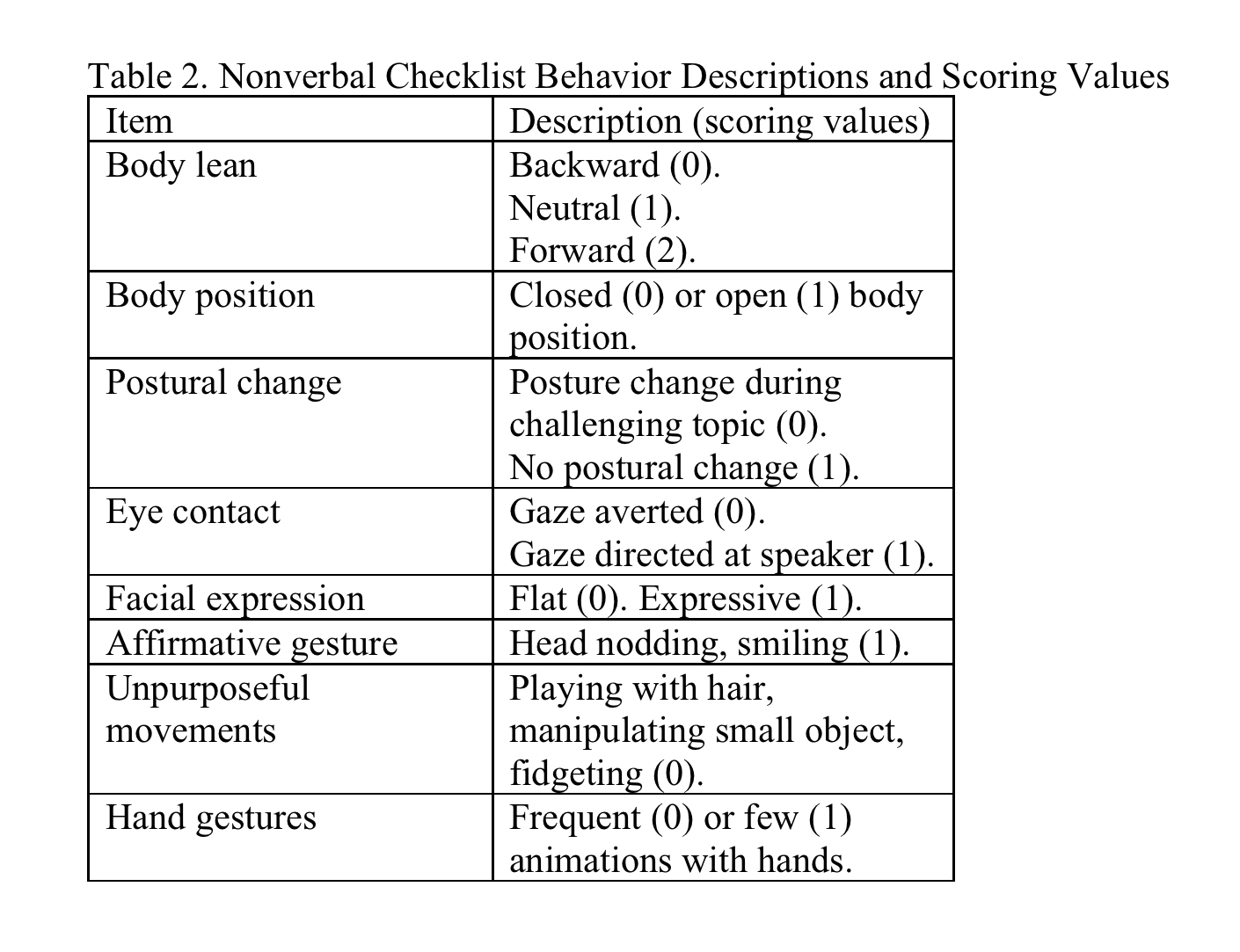
Nonverbal Checklist. Previously developed and used by Hall22 and Ishikawa,23 the Non-verbal Checklist20 (NVC) was utilized to examine non-verbal or kinetic communication in medical students during an Objective Structured Clinical Examination. Components of NVC include body lean, body position, postural change, facial expression, eye contact, affirmative gestures, unpurposive movements, and hand gestures. Table 2 defines the NVC components and scoring. With the exception of body lean, which can be scored 0, 1, or 2, components of the NVC are scored 0 or 1. Higher scores are reflective of more welcoming and approachable body language.
Readiness for Interprofessional Learning Scale. The Readiness for Interprofessional Learning Scale (RIPLS)24 is a 19-item measure designed to capture attitudes and perceptions related to interprofessional education across a 5-point Likert scale from “strongly disagree” to “strongly agree” with a maximum total score of 95. Higher scores suggest greater readiness. The general information portion of the RIPLS includes age, specialty area, and year of training. The RIPLS is made up of 4 subscales: 1) Teamwork and Collaboration; 2) Negative Professional Identity; 3) Positive Professional Identity; and 4) Roles and Responsibilities. Specifically, Teamwork and Collaboration explores the values that interprofessional members embrace and how these values impact relationships. It involves capturing findings related to communication, coordination, and discipline-specific knowledge for the purpose of learning to provide effective care as a team. The subscales of Professional Identity recognize that discipline-specific learning occurs around professional ideology and assesses the likelihood that this ideology will promote or hinder teamwork and care. Addressing learning of professional task delineation and its relevance within effective teamwork is captured in the Roles and Responsibilities subscale.24,25 Three of the 4 subscales have demonstrated good test-retest reliability.26 Negative and Positive Professional Identity can be collapsed into one subscale entitled Professional Identity.25
Intervention
Following registration into the course, students were provided the syllabus outlining course objectives and activities. During session 1, students completed consents and RIPLS, and an MUSC faculty member explained that one small group activity during each Eye Spy session would be video recorded during sessions 2 through 7. A Canon Vixia HRR500 video camera was used to video record. Following each week’s session and using the video recordings, students and museum educators scored the NVC. Students and museum educators were intentionally not educated in scoring the Nonverbal Checklist to encourage reflection rather than instruction of nonverbal behavior. Each student only reviewed and scored his or her own nonverbal behaviors. Students also commented on strengths and areas of improvement after reviewing each week’s video recording. Museum educators were assigned several specific students to review and score from the video recordings. Students and museum educators had 2 weeks to review and score the NVC before the next session. The video recordings and NVC scoring were available and managed through an online learning platform and a secure file-sharing service. Video recording did not take place during session 1 and session 8 because additional time was required for quantitative and qualitative data collection. On occasion, students had opportunities to participate in special events within the museum environment, in which video recordings were not permitted (eg, Behind the Scenes Museum tour, guest lectures by international artists). Re-administration of the RIPLS took place during the 8th and final session.
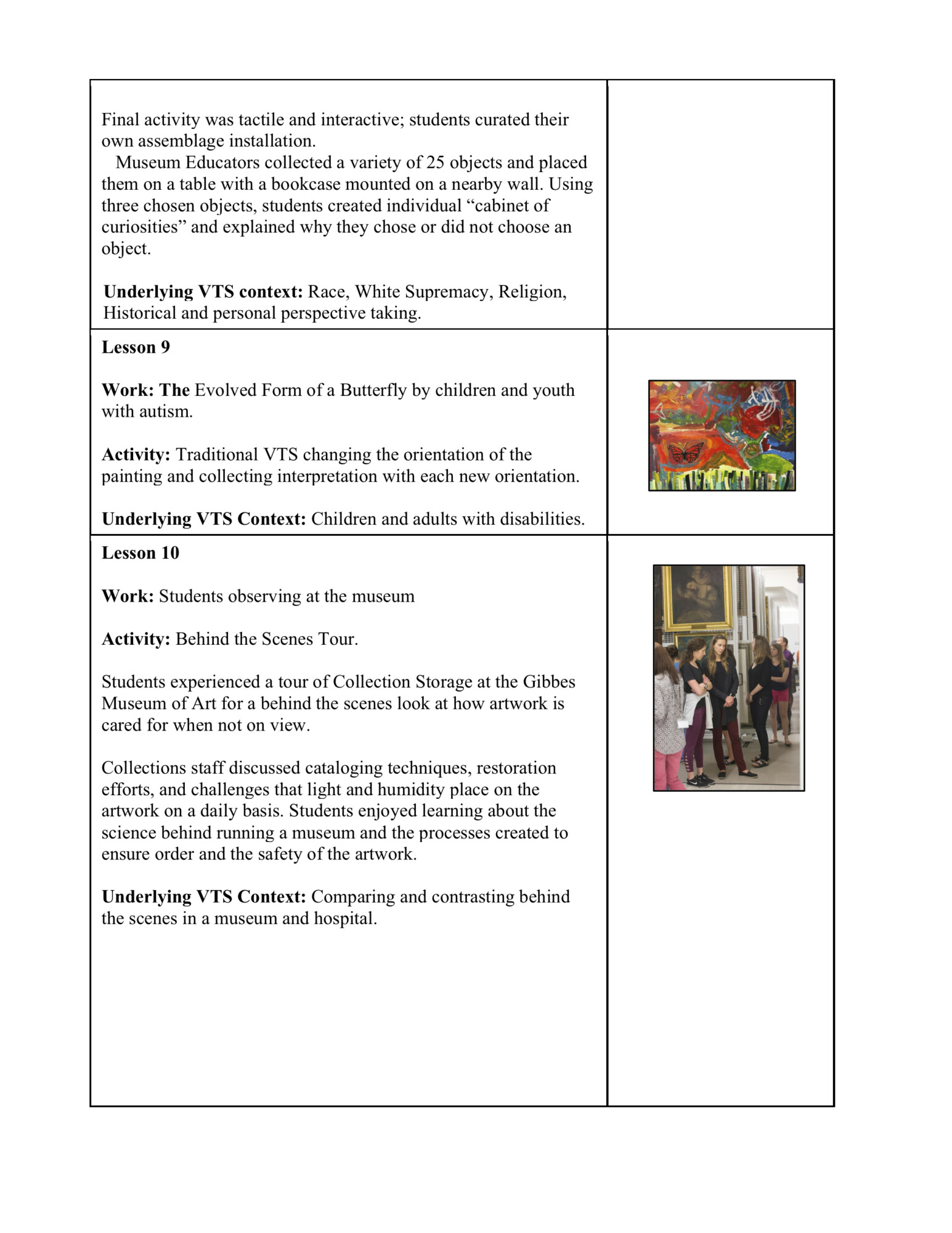
Examples of general descriptions of weekly Eye Spy lessons are available in Table 3. As can be seen from the table, lessons varied from session to session; however, in each session excluding special events, students were involved in 1 large and 2 small group lessons over 2 hours, facilitated by museum educators and faculty members. Small and large group lessons were grounded in the VTS pedagogy, yet scaffolded across sessions to build affective domain development.
Sessions 1 and 2 were designed to establish rapport and create general familiarity with VTS inquiry. In one early session, for example, using a painting entitled 502 Lucerne Street by Edward Rice, students participated in an open discussion offering many different perspectives that led to multiple interpretations. Subsequent sessions consistently targeted communication and observation skills, but also sought to impact and advance affective development toward valuing, organization, and characterization. In this case, students advanced affective skills involving valuing by unraveling the hidden messages and emotions held within the multimedia work entitled The Evolved Form of a Butterfly that was created by a diverse sample of children living with autism spectrum disorder.
Results
Nonverbal Checklist
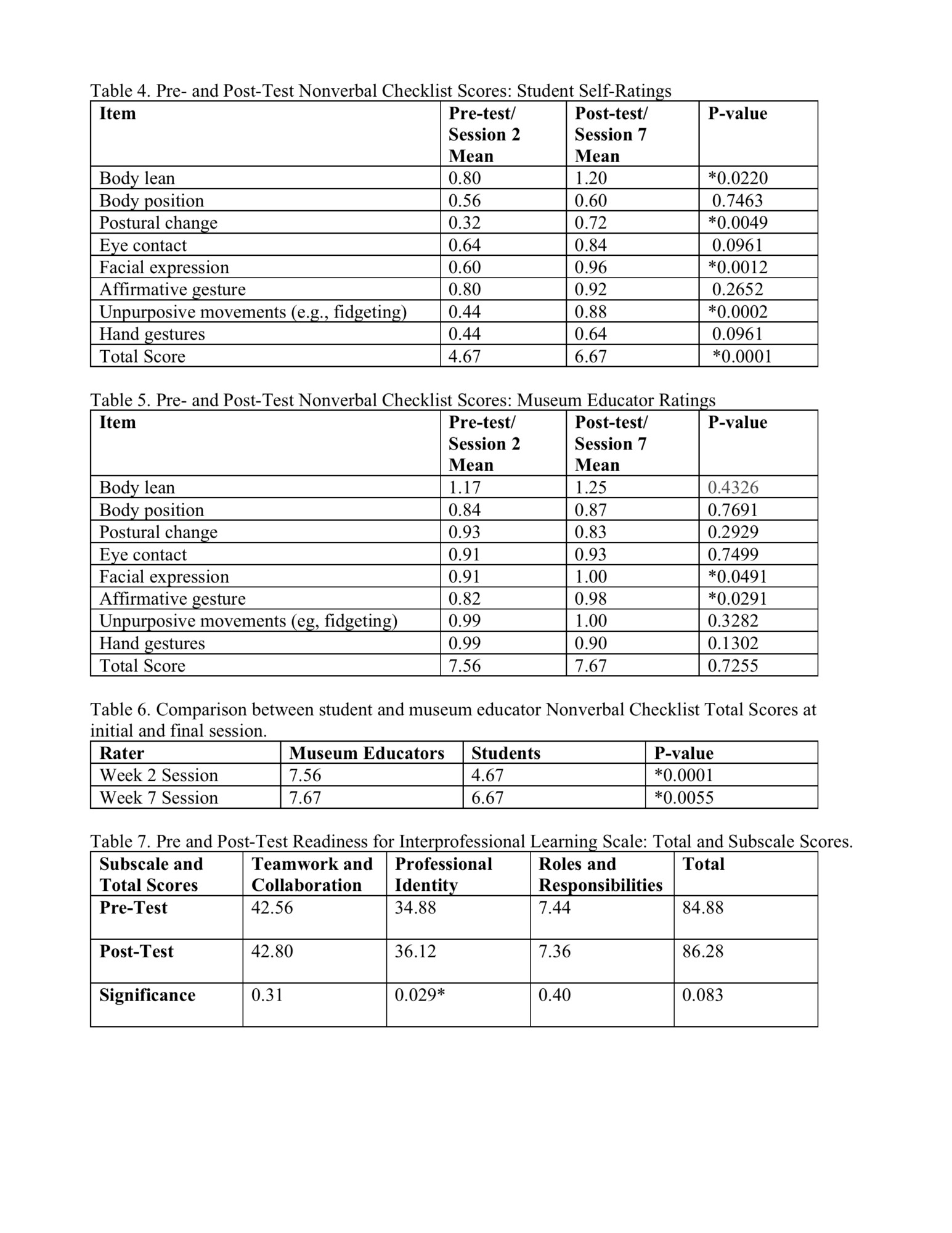
All analyses were conducted using SAS version 9.4 (SAS Institute, Cary, NC), with two‐sided statistical significance set a priori at P < 0.05. Paired t-tests were used to compare NVC group mean scores from the first (session 2) to last (session 7) session video-recordings, rather than the planned repeated-measures analysis of variance. This is because the majority of students missed one session secondary to clinical educational duties, and absences varied across session weeks, which annulled the repeated-measures statistical testing. Eleven student absences occurred across eight sessions. All students were present for sessions 2 and 7; therefore, statistical testing with a paired t-test was carried out for these sessions. Significant improvements were displayed in the Total and 4 item scores on the NVC as measured by student self-ratings. The museum educators’ ratings for 2 NVC item scores improved significantly. Only the Facial Expression item significantly improved for both students and museum educators. Tables 4 and 5 display Nonverbal Checklist values from student and museum educator ratings. Comparative ratings between the students and museum educators at session 2 and 7 timepoints were significantly different (Table 6).
Readiness for Interprofessional Learning Scale
Paired t-tests were used to compare group mean scores from the first session (1) to last session (8). Table 7 displays the total and three subscale scores for the Readiness for Interprofessional Learning Scale. The Professional Identity subscale was significant (p=0.029) as was the Professional Identity subscale item labeled “Shared learning and practice will help me clarify the nature of patients’ or clients’ problems” (p=0.0005). Improved trends were noted for the Teamwork and Collaboration subscale and Total scores, but were not significant.
Discussion
Nonverbal Communication Skills
Following use of VTS within a museum environment and at the affective domain foundational levels, interprofessional students demonstrated improvements in nonverbal behaviors. The characteristics of receiving and responding are well represented within the NVC (eg, nodding affirmative action, leaning in or away, eye contact) and their associated improvements positioned students for advancement into valuing, organization, and characterizations. These higher-level affective characteristics were not directly measured quantitatively; however, student comments on their NVC behaviors suggest that preliminary improvements in the more advanced areas of the affective domain were occurring. Below, we provide student comments demonstrating potential gains into higher levels of the Bloom’s affective domain.
- Valuing: Inclusion and diversity theme: “This exercise was interesting for me because I interpreted a different scene in the piece than the direction the rest of the class was taking it. I originally wasn’t going to speak up, but the facilitator made sure to get every opinion from the group. Next time I should still voice my opinion even if it is opposite from the majority of the group.”
- Organization: Responsible for one’s behavior theme: “I could learn to voice my disapproval of connotations & not be afraid of what others may think because my opinions are mine & theirs are allowed to differ (if they do). I should practice with uncomfortable conversation topics.”
- Characterization: Value-guided behavior theme: “I would like to have a smile on my face more often, however the topic [Requiem for Mother Emanuel] we were discussing did not warrant a smile, so maybe I will look different next time. Since we were discussing art, I think that my emotions were removed from the situation. I understand this is a very sensitive topic and I do have sympathy for the ones lost and their families. I think that in a situation when I am interacting with another person and it requires compassion, that I do a better job of expressing my sympathy and compassion.”
These comments reflect trends in the construction of students’ awareness and understanding of others’ perspectives, thereby providing a self-reflective lens through which students recognize their implicit knowledge and behaviors and take the opportunity to build one’s value system and act in a value-guided manner.
Differences in NVC scoring between students and museum educators existed. Students clearly critiqued their nonverbal behaviors more stringently than museum educators. For the museum educators, a ceiling effect in the initial NVC scores was noted, so little subsequence change occurred at the final scoring. Several possibilities exist for this lack of change. The museum educators involved with this course often spent much of their time educating primary school children. The opportunity to work with adult graduate students may have been more intellectually stimulating and inflated their perception of students. In addition, since no formal instruction concerning the NVC was provided to encourage reflection of nonverbal behaviors, the museum educators may have misinterpreted the scale, and consequently, scores were elevated.
Perception of Interprofessional Practice
With pre- and post-total RIPLS scores equaling 84.88 and 86.28 out of 95 respectively, once again a ceiling effect is noted for students participating in this course. The MUSC is committed to interprofessional (IP) education and practice. At MUSC, all first-year students across 6 colleges and multiple programs are required to participate in a 4-week course devoted exclusively to interprofessional learning. Additionally, each year for one full day in January, the University cancels classes across all colleges and requires all students to participate in interprofessional exercises for what is titled IP Day. This extensive introduction to IP learning and practice may explain the total RIPLS score ceiling effect and lack of change. Comparisons between this study’s high RIPLS pre- and post-test total scores of 84.88 and 86.28 out of 95 to other IP studies support this conclusion. For instance, Janotha and colleagues22 reported RIPLS mean post-test scores of 78.3 following an IP clinical experience between dental and nurse practitioner students. A similarly lower RIPLS mean post-test score of 75.02 was reported by Walker and colleagues23 following placement of undergraduate healthcare students in rural clinics.
Although the total RIPLS score did not demonstrate significant improvement, the significant improvement in the RIPLS Professional Identity subscale and “Shared learning and practice will help me clarify the nature of patients’ or clients’ problems” item is interesting and may indicate advancement of affective domain development. This RIPLS subscale is reflective of defining one’s professional identity and professional contributions to an IP team. For a team to promote inclusive, diverse, and balanced awareness and decisions, each team member must recognize communication and perspective-taking skills are necessary. This recognition supports ascension toward valuing and organization within the affective domain. Future museum-based VTS studies involving IP education and practice with the goal of specifically targeting higher levels of the affective domain, such as inclusion, diversity, and implicit biases, would most likely prove constructive.
Framing Future Studies
As previously highlighted, the majority of studies examining the effects of museum and art-based instruction have occurred involving medical students; a gamut of various outcomes has been explored, from communication, ambiguity, and reflection to empathy. Similar to how traditional health science outcomes and interventions are mapped and evaluated across the International Classification of Functioning, Disability and Health, the authors of this paper would suggest that conceptualizing and organizing outcomes and instructional strategies for future studies across the framework of the affective domain would promote clearer understanding of the possible hierarchical nature of affective student learning, strengthen museum and art-based instruction evidence, identify gaps in the evidence, and guide future research directions. Consider the work of Gowda and colleagues,15 which noted significant improvement in medical students’ reflective ability, but not for personal bias and tolerance for ambiguity. Is this lack of improvement secondary to the need for lower affective domain development before higher-level attainment can be achieved?
Ultimately, our study authors suggest that in order to ensure that all future healthcare providers are compassionate and patient- and family-integrated, essential instruction in the development of lower affective skills followed by the intentional targeting of higher affective levels is necessary. Although results from our study provide preliminary evidence that museum-based instruction can lead to improvement in interprofessional learning and nonverbal communication, much more educational research about affective instruction and development is needed. Prospective randomized controlled trials and longitudinal study designs—to establish whether affective domain development following museum- and art-based instruction in health science education leads to the actualization of compassionate patient- and family-integrated care providers within clinical settings—would be of great value to the field of health science education.
Limitations
This study suggests improvements in affective domain development of health science students, but there are factors that may have generated biases and limited interpretation of results. The Eye Spy course is an elective interprofessional opportunity within MUSC. Twenty-four of the 25 students self-selected to participate, undoubtedly leading to self-selection bias. Because the principal investigator appointment was within the College of Health Professions, Division of Physical Therapy, participant recruitment was more easily solicited and therefore enrollment was greater for this college.
Additionally, our sample lacked racial diversity, with 92 percent of participants being white. In future investigations, greater participant heterogeneity would provide broader perspective insight and most likely lead to improved affective development across the student cohort. Although only 11 absences were missing from data collection and analyses, museum-based events interfered with the initial study design and resulted in data collection reductions. The design of future studies should remain constant or special event opportunities should be built into the design. Student participants in years of study with greater clinical demands recorded most absences; therefore, enrollment consideration as to the year of health science study may need to be considered. At the intervention level, the authors would suggest that video recording is carried out without student awareness. Because students could see that the video recording was occurring, there is a question as to the genuine quality of their nonverbal behaviors. Taking steps to minimize students’ awareness during video recording may enhance confidence in the authenticity of nonverbal behaviors. Also, future studies may consider professional videography that provides a quality video recording as this may enhance visualization of nonverbal behaviors from which participants and museum educators score. This study intentionally did not educate participants and museum educators in the NVC, in order to encourage self-reflection rather than nonverbal instruction. Future researchers may wish to provide this education, as this may lead to different findings and interpretations.
Conclusion
This study is one of the first to involve an IP group of health science students exploring affective domain development using a VTS intervention in a museum-based setting. Quantitative findings indicated improvements in nonverbal communication skills and enhanced perceptions of interprofessional practice in health science students. Future health science educational studies involving humanities and targeting outcomes and interventions across the various levels of the affective domain are needed to support the development of compassionate and patient- and family-integrated care providers.
References
- Trzeciak S, Mazzarelli A. Compassionomics: The Scientific Evidence that Caring Makes a Difference. Pensacola, FL: Studer Group; 2019.
- Bloom BS, Engelhart MD, Furst EJ, Hill WH, Krathwohl DR. Taxonomy of educational objectives: the classification of educational goals. Handbook I: Cognitive domain. New York: David McKay Company; 1956.
- Anderson LWK, David R. . A taxonomy for learning, teaching, and assessing: A revision of Bloom’s taxonomy of educational objectives. New York: Longman; 2001.
- Krathwohl DR, Bloom BS, Masia BB. Taxonomy of educational objectives, the classification of educational goals. Handbook II: Affective domain. New York: David McKay Company; 1964.
- Wilson LO. The Second Principle. http://thesecondprinciple.com/instructional-design/threedomainsoflearning/. Published 2017. Accessed2017.
- Wershof Schwartz A, Abramson JS, Wojnowich I, Accordino R, Ronan EJ, Rifkin MR. Evaluating the impact of the humanities in medical education. Mt Sinai J Med. 2009;76(4):372-380.
- Klugman CM, Peel J, Beckmann-Mendez D. Art Rounds: teaching interprofessional students visual thinking strategies at one school. Acad Med. 2011;86(10):1266-1271.
- Charon R. Narrative Medicine: Attention, Representation, Affiliation. Narrative. 2005;13(2):261-270.
- Charon R, Hermann N, Devlin MJ. Close Reading and Creative Writing in Clinical Education: Teaching Attention, Representation, and Affiliation. Acad Med. 2016;91(3):345-350.
- Yenawine P. Visual Thinking Strategies: Using art to deepen learning across school disciplines. Boston, MA: Harvard Education press; 2013.
- Lown BA. A social neuroscience-informed model for teaching and practising compassion in health care. Med Educ. 2016;50(3):332-342.
- Costa MJ, Costa P. Nurturing empathy and compassion: what might the neurosciences have to offer? Med Educ. 2016;50(3):281-282.
- Haidet P, Jarecke J, Adams NE, et al. A guiding framework to maximise the power of the arts in medical education: a systematic review and metasynthesis. Med Educ. 2016;50(3):320-331.
- Miller A, Grohe M, Khoshbin S, Katz JT. From the galleries to the clinic: applying art museum lessons to patient care. J Med Humanit. 2013;34(4):433-438.
- Gowda D, Dubroff R, Willieme A, Swan-Sein A, Capello C. Art as Sanctuary: A Four-Year Mixed-Methods Evaluation of a Visual Art Course Addressing Uncertainty Through Reflection. Acad Med. 2018;93(11S Association of American Medical Colleges Learn Serve Lead: Proceedings of the 57th Annual Research in Medical Education Sessions):S8-S13.
- Katz JT, Khoshbin S. Can visual arts training improve physician performance? Trans Am Clin Climatol Assoc. 2014;125:331-341; discussion 341-332.
- Pellico LH, Friedlaender L, Fennie KP. Looking is not seeing: using art to improve observational skills. J Nurs Educ. 2009;48(11):648-653.
- Understanding Team STEPPS Guide and Team STEPPS Pocket Guide. https://www.aha.org/center/performance-improvement/team-training/resources Published 2020. Accessed2020.
- Kohn L. To err is human: an interview with the Institute of Medicine’s Linda Kohn. Jt Comm J Qual Improv. 2000;26(4):227-234.
- Collins LG, Schrimmer A, Diamond J, Burke J. Evaluating verbal and non-verbal communication skills, in an ethnogeriatric OSCE. Patient Educ Couns. 2011;83(2):158-162.
- Naghshineh S, Hafler JP, Miller AR, et al. Formal art observation training improves medical students’ visual diagnostic skills. J Gen Intern Med. 2008;23(7):991-997.
- Hall JA, Harrigan JA, Rosenthal R. Non-verbal behaviour in clinician-patient interactions. Appl Prevent Psycho. 1995;4:21-37.
- Ishikawa H, Hashimoto H, Kinoshita M, Fujimori S, Shimizu T, Yano E. Evaluating medical students’ non-verbal communication during the objective structured clinical examination. Med Educ. 2006;40(12):1180-1187.
- McFadyen AK, Webster V, Strachan K, Figgins E, Brown H, McKechnie J. The Readiness for Interprofessional Learning Scale: a possible more stable sub-scale model for the original version of RIPLS. Journal of interprofessional care. 2005;19(6):595-603.
- Parsell G, Bligh J. The development of a questionnaire to assess the readiness of health care students for interprofessional learning (RIPLS). Med Educ. 1999;33(2):95-100.
- McFadyen AK, Webster VS, Maclaren WM. The test-retest reliability of a revised version of the Readiness for Interprofessional Learning Scale (RIPLS). Journal of interprofessional care. 2006;20(6):633-639.
About the Author(s)

Cynthia Dodds, PT, PhD
Cynthia Dodds, PT, PhD is an Associate Professor at the Medical University of South Carolina. She regularly implements humanities instructional strategies into physical therapy education to enhance affective development of students. Her current project entitled Eye Spy for Development of Affective Qualities in Interprofessional Healthcare Students has South Carolina Clinical and Translational Research Team Science funding to examine students’ communication and observation skills within a museum setting.

Brooke Mulrenin, OTR/L, MS
Brooke Mulrenin, OTR/L, MS is a pediatric occupational therapist and Ph.D. candidate studying Health and Rehabilitation Science at the Medical University of South Carolina. Her current research involves improving measurement of infant feeding and swallowing disorders. Through research and teaching, she hopes to promote compassionate, family-centered approaches to feeding, allowing mealtimes to be a source of enjoyment and connection. As a graduate assistant for the Eye Spy course, Brooke gained immense appreciation for the value of art- and humanities-based instruction, observing that together, educators and students created an environment of trust that fostered uncommonly generous listening and sharing. She believes this type of learning experience provides space to honor the complexity of being human and to develop patience to work through difficult realities — important practices for health science students and health professionals.

Carrie Cormack, DNP, APRN
Carrie Cormack, DNP, APRN is an Assistant Professor at The Medical University of South Carolina. She is the lead Palliative Care faculty in the Doctor of Nursing Practice program. Carrie moved to South Carolina as a new graduate Registered Nurse to follow her dreams of working in Pediatric Nursing. Now, with over 20 years’ experience in Pediatric Nursing, she has worked in acute care, Developmental Pediatrics, Pediatric Orthopaedics, as the Director of Nursing at a school for children with severe and multiple disabilities, and with a community based palliative care organization. She continues to specialize in palliative care and, in addition to her faculty work, she practices as a pediatric nurse practitioner with the Pediatric Palliative Care team at the Shawn Jenkins Children’s Hospital in perinatal palliative care at MUSC. Certified by the Pediatric Nursing Certification Board and the Hospice and Palliative Nurses Association, Carrie is dedicated to increasing palliative care education as well as the humanities education in nursing programs. She is committed to empowering students to better understand, relate to, and care for their patients and families, especially those with serious illness.

Kimberly Kascak, MS
Kimberly Kascak, MS is an Assistant Professor at the Medical University of South Carolina (MUSC). She has a background in special education, medical education, academic innovation, and online instructional design in the field of education. She has worked collaboratively with interprofessional teams including but not limited to physical therapists, occupational therapists, speech therapists, nurse practitioners, families, and educators throughout my career. She has developed and coordinated innovative online academic programs with continual ongoing educational support to programs. Her current focus involves collaborative, interprofessional, and online instruction. As a certified TeamSTEPPS Master Trainer, she provides instruction to MUSC students through required interprofessional courses.

Rebecca “Becca” Hiester
Rebecca “Becca” Hiester is the Director of Education and Programs at the Gibbes Museum, where she oversees all educational programs for K-12 and adult audiences, including all collaborative programs between the Gibbes and the Medical University of South Carolina. A Charleston native, she has an MA in art history from the University of Massachusetts, Amherst and a BA in anthropology and art history from Wake Forest University. She volunteered as a Museum Educator and with the curatorial department at the Gibbes for five years before becoming a Curatorial Assistant in 2014. She is currently pursuing a Masters of Library and Information Science with the University of South Carolina in addition to working full time with the Gibbes.
![]()
This work is licensed under a Creative Commons Attribution 4.0 International License.