Community Mobility Method Selection in Individuals With iSCI: A Qualitative Analysis
doi: 10.18737/0607516672
AMA Citation: Holleran CL. Community Mobility Method Selection in Individuals With iSCI: A Qualitative Analysis. J Hum Rehabil. 2021; Fall. doi:10.18737/0607516672
Table of Contents
Background: A primary rehabilitation goal for individuals with motor incomplete spinal cord injury (iSCI) is to regain walking abilities and return to community-level ambulation. Outside of quantitative indicators, little evidence exists to inform therapists in assisting patients in navigating community mobility method decisions.
Objectives: Describe the factors included in the choice between walking or using wheeled mobility methods in the community for individuals with motor iSCI who have the capacity to walk.
Design: A qualitative, grounded theory design was used to address the study aim.
Methods: Seven individuals of varying chronicity and physical capacity with iSCI participated in one-on-one semi-structured interviews. Interviews were recorded, transcribed, coded, and organized into themes and subcategories to develop the theory of how individuals make mobility method decisions.
Results: Individuals with iSCI described the factors they consider when choosing to walk, use wheeled mobility, or avoid community mobility altogether. Informants described a process of planning before any community outing that considered assessment of their body structures and functions, the task demands, and the environmental barriers and facilitators. Their perspectives on disability also influenced their mobility method choices.[/vc_column_text][vc_column_text]
Introduction
There are 12,000 reported cases of spinal cord injuries (SCI) in the United States each year.1 Incomplete injuries, indicative of sensory or motor sparing below the level of the injury, are becoming more prevalent.2 A primary rehabilitation goal for individuals with motor incomplete spinal cord injury (iSCI) is to regain walking abilities.3 While many individuals with iSCI have the goal of independent walking, clinicians early in the rehabilitation process (ie, inpatient rehabilitation) must balance therapy time between restorative walking interventions and training for functional independence in activities of daily living upon discharge. Further, discharge preparation includes the prescription of durable medical equipment for safe functioning in the home and the community. Apart from quantitative indicators, there is a paucity of qualitative information from individuals with spinal cord injury describing the factors that influence the selection of community mobility modes and devices. A deeper understanding of these factors could allow therapists to deploy more patient-centered care.
Characteristics: a Multitude of Factors
The characteristics of individuals who describe themselves as community ambulators have not been fully explored. The quantitative characteristics of these individuals have been described in separate cohorts with the use of body structures and function assessments (individual’s impairments), capacity measures (what the individual’s walking ability is), and performance assesments (how much the person walks in the real world).4 Perry et al5 described individuals that self-report community ambultation demonstrated walking speeds exceeding 0.4 m/s.5 Saraf et al6 provided discriminative capacity and performance values in a cohort of individuals with motor iSCI that described themselves as completing some walking in the community as those who walked at > 0.35m/s (meters per second) on the 10-meter walk test (capacity measure), >140m (meters) during the 6-minute walk test (capacity measure), or participated in >2200 total steps per day (performance mesaure) as measured by an accelerometer.6 Body structure and function characteristics such as quadriceps strength,7,8 hip flexor strength,6 gait efficiency,9 age,10 balance,6 upper-extremity strength,11 and gait speed12 have been correlated to walking capacity, with conflicting reports of the role of spasticity on walking capacity.6,7,10,12,13
However, utilizing solely quantitative factors to determine who will walk in the community likely excludes a multitude of other factors that individuals consider when navigating mobility-related choices. Spinal cord injury results in impairments in the motor and/or sensory systems in the upper and lower extremities, trunk, and pelvic region, to varied degrees.14 These impairments can alter the physical appearance of the human body and an individual’s function and independence,15-17 leading to disability.
The definition of disability varies depending on the model used to describe the concept. The World Health Organization’s International Classification of Function, Disability and Health (WHO-ICF), an enablement model used in rehabilitation, defines disability as “a complex phenomenon that is both a problem at the level of a person’s body, and a complex and primarily social phenomenon.”18 The social model of disability, championed through both the disability rights and independent living movements, frames disability as a normal part of the human experience.19 This model emphasizes the attitudinal, structural and social barriers that limit individuals in achieving their life goals, with the discriminatory view society has toward individuals who experience disability as the primary barrier.19
Data from separate cohorts of individuals who have experienced disability details how the experience of disability can either positively20 or negatively affect an individual’s sexual identity,21 self-esteem,22 gender roles,23 body image,24 and views on self-presentation.25 Self-presentation is behavior that attempts to convey information about oneself or an image of oneself to other people.26 A qualitative analysis by Bailey et al25 explored the body image experiences of people with spinal cord injury and found that individuals reported the use of differing self-presentation strategies to manage stigma associated with having a disability, including the use of a wheelchair. Another analysis by Jannings et al27 reported that individuals with spinal cord injury experienced negative reactions from individuals in the community based on their physical disability. It is unclear how individuals with spinal cord injury make decisions regarding future stigma when making mobility-related decisions.
Factors Affecting Choice
Therefore, the purpose of this study was to explore the factors individuals with motor incomplete spinal cord injury, who have the capacity to walk, consider when choosing community mobility methods.
Methods
Informants were purposefully selected from a larger quantitative study examining correlates of community mobility in individuals with chronic motor iSCI. Inclusion criteria for the quantitative arm of the study included individuals aged 18 to 75 years with a history of traumatic or non-traumatic, non-progressive motor incomplete American Spinal Injury Association (ASIA) impairment classification of C or D; injury incidence >1-year duration; neurological levels C1-T10; and the ability to ambulate >10 meters. Individuals with concurrent severe medical illness, pre-existing osteoporosis, history of other peripheral or central neurologic injury, and history of significant obstructive and/or restrictive lung diseases were excluded. Additional exclusion criteria included receiving physical therapy, experiencing a change in medical status, or changing medications over the 30 days prior to enrollment.
Study Design
Informants’ gait speed was evaluated with the 10-meter walk test as a part of the larger quantitative study from which they were recruited. Predictive walking categories described previously by Perry et al5 were utilized for purposeful sampling. Perry categorizes individuals who perform full community ambulation as those who walk >0.8 m/s; those who perform limited community ambulation, as those who walk 0.4-0.8 m/s; and those who perform household or no ambulation, as those who walk <0.4 m/s.5 The primary researchers (CLH & JLF) purposefully selected individuals from each of the three gait categories to gain a comprehensive understanding of the factors that impact mobility-method selection from persons with differing ambulatory abilities. Constant comparative analysis provided the researchers the ability to collaborate after open coding of each interview to determine the criteria for the next informant. In addition to selecting individuals who had differing ambulatory capacities, the researchers also sampled individuals with diverse chronicity post-SCI, levels of injury, socioeconomic backgrounds, and type of home community (rural or urban). The researchers selected subsequent informants after each interview in an attempt to continually challenge theme-building, and to allow for generation of a theory that was more likely to be transferred to the greater population of individuals with iSCI.
Data Collection
Grounded theory methodology was selected for this analysis to provide an in-depth investigation of the factors considered by individuals with chronic motor iSCI to utilize either walking or wheeled mobility methods in the community. Informants engaged in semi-structured interviews that occurred in a private setting. All data was transcribed and coded after each interview to incorporate a central feature of grounded theory—the constant comparative method.28-30 Field notes were taken to incorporate informants’ non-verbal communication throughout the interviews as part of the analysis, and memos were maintained throughout the coding process to enhance confirmability. An initial outline of questions was constructed prior to the first interview and is provided in Table 1. Questions were developed to explore how individuals made the choice between walking and using a wheelchair in the community from a variety of angles, and were designed to explore each individual’s experiences with community navigation. Questions were designed to be open-ended; however, the researcher asked additional questions (eg, “Could you tell me more about…?”) based on information that was revealed throughout. The primary researcher (CLH) recorded personal biases prior to and concurrent with data collection and analysis to demonstrate reflexivity. This project was approved by the Northwestern University Institutional Review Board and the University of Indianapolis Institutional Review Board. All informants participated in written informed consent.
Data Analysis
Interviews were recorded and transcribed verbatim by the primary researcher. No identifiable information was utilized within the interview. Coding for grounded theory has been described by Strauss and Corbin as occurring in three stages: open-coding, axial coding, and selective coding.29 During open-coding, the primary researcher and a second researcher (JF) independently coded the data from each interview line by line, identifying in-vivo codes that closely matched the informants’ own words. Subsequently, researchers collaborated to verify initial codes, thus providing reliability of results while further reducing researcher bias.31 Constant comparative analysis occurred as the researchers compared new information to codes identified from previous interviews, with all decisions maintained in a codebook. The researchers continually built upon previous codes, eliminated codes, or established new codes throughout the analysis. This process also allowed the researchers to determine when data saturation was achieved, meaning no additional interviews were required to develop the theory.
The researchers met regularly to re-evaluate emerging codes and to continually sort and analyze the data. After the fourth interview, axial coding was initiated as themes began to emerge. Large amounts of data were synthesized, sorted, compared to one another, and were reorganized continually. Similar codes were grouped together and labeled with a more global conceptual theme. This included both positive and negative comments that related to the theme. After the sixth interview, the researchers independently re-read all transcripts, and reviewed existing themes to ensure preliminary themes were representative of the data. Selective coding occurred as researchers defined, developed, and refined the themes and began to build the theory. At this time, a third researcher (SCM), with clinical expertise working with persons with neurologic disease or injury, was consulted. This researcher reviewed all data and the preliminary themes to ensure dependability of results, and assisted with the theory development. Subsequently, all three researchers concluded that an additional interview was required to ensure saturation of data. Saturation in this analysis was determined when no additional data captured would support further development of the themes, as similar instances are occurring repeatedly.32
After the seventh interview, all three researchers agreed saturation had been achieved and all researchers confirmed the theory of how individuals with spinal cord injury choose methods for community mobility. After the theory was developed, the primary researcher met with a focus group that included four informants to verify theory and themes to ensure dependability of the data.25 Additionally, the results were presented to a panel of clinicians—two physical therapists and one occupational therapist with greater than one-year experience working with individuals with chronic motor iSCI. This step provided data triangulation, an essential element of grounded theory development, to ensure dependability and credibility of results based on each clinician’s interactions with the population under study in navigating community mobility choices.31
Results
Interviews lasted approximately 20 minutes to an hour. Individual demographic data including age, length of time post-spinal cord injury, neurologic level of injury, sex, gait speed, lower-extremity motor scores (LEMS), upper-extremity motor scores (UEMS), and durable medical equipment device use, are provided in Table 2. All informants had established multiple options for community mobility (ie, multiple devices to support either walking or wheeled mobility) that were informed by an analysis of their body function and structures, frequently encountered environmental factors, and the task demands required to navigate their individual community mobility goals. Separate from the interaction of these factors, each informant expressed their perspective on disability as being influential in choosing primary methods of community mobility. Informants were in varied chronicity after their injury, and each spoke of this ongoing analysis since their injury. Therefore, each individual’s mobility mode and supportive equipment were evolving with both time and the lived experience of disability.
Figure 1 depicts the interaction of the two primary themes, and the iterative analysis that each informant described when navigating ongoing community mobility method selection. Two main themes emerged: (1) interaction of the environment, task demands, and body function and structure characteristics; and (2) perspectives on disability.
Interaction of Environment, Task Demands, and Body Function and Structure Characteristics.
All informants described a process of planning prior to selecting a mode of community mobility, as all individuals had established more than one mobility option to navigate the community. Informants considered these three primary factors and the risks associated with each. Included were: (1) the environments encountered during a community outing; (2) the task demands; and (3) the individual’s body structure and function characteristics at the time of community mobility, as well as the changes to those body structure and function characteristics anticipated for the duration of the community outing.
Environments Encountered During a Community Outing. Informants considered the environment in which the community mobility tasks would occur. Environmental factors or conditions such as weather, accessibility, and terrain were described as factors affecting their mode selection. Informants reported weather was a factor and often a deterrent to community mobility. Informants shared that weather such as rain, ice, or snow could affect the safety and increase the risk of participating in community mobility, especially when walking. The interaction of weather and body function and structure characteristics was also discussed. Some informants described that weather (eg, cold or wind) could alter their body function and structure characteristics such as their tone, strength, or fatigue levels, among others. One informant described;
“So if it’s snowing or raining, um, traction is difficult for me, steps are particularly dangerous for me. I move very slowly, so in rain—and I can’t carry an umbrella— so it might be likely that I get soaked instead of staying dry, so you know that may keep me out, for instance. So the weather really is a factor of whether or not I would even get out in the community.” [Informant 1]
Community accessibility (or lack thereof) was also an environmental consideration for mobility method selection. This included accessibility of transportation as well as all environments encountered within the community outing. Informants shared:
“I started to realize that all stores are not wheelchair-friendly.” [Informant 2]
“…most restaurants aren’t really accessible.” [Informant 5]
“with a wheelchair in a restaurant, you know, sometimes the table doesn’t fit.” [Informant 7]
“….you need so many accommodations to use the power chair [in the community].” [Informant 4]
Informants also described how the varying environments (eg, terrain) encountered within community mobility could change the demands of the task, thereby linking the environmental features and task demands.
Task Demands. Informants described careful consideration of the demands of the community activity, including all elements of each task. This included the distance requirements, amount of standing, available sitting surfaces, the time available to complete all components, and how each of these factors would affect the individual’s physical state if either walking or using wheeled mobility. Informants also considered how they wanted to interact socially during these community outings, and how their choices of mobility method would affect the amount of energy they had to interact socially.
Some expressed that they would be “too tired” [Informant 2] when they got to their destination if they walked, or shared that it was “hard [for me] to have a real long conversation [while walking]” [Informant 6]. Many expressed that if it required too much effort to go a given distance in the given amount of time, then they might choose wheeled mobility for increased efficiency and safety.
Informants also considered transportation in relationship to the task demand and the type of transportation available in their local community. All the informants spoke of the difficulty of transportation with a wheelchair, especially powered wheelchairs. Even though transportation accessibility is an environmental consideration, informants also spoke of accessibility in relation to the task demands. They considered the effort it took to transport (eg, break down, lift into car, bring extra batteries, etc.) a wheelchair. For example, some informants described changing their mode of transportation (ie, taking the bus) in order to have their power wheelchair during the task, while others chose to walk, as powered wheelchair transportation was cumbersome.
Informants further described calculating the risks of choosing to navigate the task demands either by walking or using a form of wheeled mobility. Heavily influential in their decision of how they could navigate those task demands was their body function and structures at the time of a community outing, and the anticipated changes over the course of community mobility with their body function and structures.
Body Function and Structure Characteristics. Informants’ body function and structures, such as strength in the upper and lower limbs, heavily weighted into the decision to walk or use a particular form of wheeled mobility. For some, although they had the capacity to walk, they had inadequate cardiorespiratory fitness to navigate community-level distances. Informants described consideration of a variety of body functions and structure characteristics including strength, bowel and bladder function, motivation, upper-extremity function, fatigue, pain, and spasticity—both prior to, and during the anticipated fluctuation of, these faculties—over the duration of any community mobility outing. Their assessment of the current state and future predicted state (based on task demands and environment) affected their mobility choices.
Many informants specifically described the importance of upper-extremity function and fatigue when deciding between differing forms of wheeled mobility, which related to type of transportation. For many informants, the fact that they had tetraplegia made manual wheelchair propulsion and wheelchair breakdown into a car difficult or unattainable. Informants spoke of how decreased upper-body function made manual wheelchair propulsion inefficient, which resulted in them choosing between walking or power wheelchair mobility (either motorized powered or push-rim activated power assist wheels on a manual wheelchair frame). Many informants also described their fear of the negative factors associated with prolonged sitting as it related to wheelchair use. Two informants described this complex calculation of their body function and structure characteristics, the task demands, and environment, stating:
“Being a functioning quad, and my lack of arm, finger, and upper-body strength also made wheeled mobility an inconvenient option in terms of solo travel in a vehicle. So it would have limited me more towards van transportation because I am unable to pick up the chair and really having trouble moving the chair forward; therefore, my option was really the power chair, which would have been terrific except for all the consequences of sitting that long. I was more willing to take the risks of learning how to walk. I’m prone to falls, balance issues, but I think that, in my humble opinion, offsets the risks of long-time sitting, potential pressure issues, cardiovascular health, and just mental health for me.” [Informant 7]
“I always think about the entire round trip. So where am I going, how long am I going to be there, and then when do I come back? I relate that back to my bladder; where am I going, what’s the washroom situation going to be, how long am I going to be there, what have I drank like the last two hours before I left; …with the weather, am I gonna have difficulty on my own, will the weather affect my tone, is it going to be cool, excessively windy? Like, I get touch sensitivity, so if there is a lot of wind, I can get tone. Where I am going to, I like to know what I am getting myself into; so, is there [a] stair where I’m going, is it handicapped accessible? Who is going to be there that kind of understands my situation that I can rely on them if I need them? If I am going with my girls, what kind of atmosphere is it going to be? Am I going to be anxious because I have to keep an eye on them and then manage my own self?” [Informant 1]
Perspectives on Disability and Mobility Choice
Informants expressed their perspectives on disability and their perceptions of how individuals in the community reacted to them when using differing forms of mobility. Each informant had a unique perspective of how a mobility method related to his or her identity, how others would perceive that identity, and how this influenced their self-presentation. Some described that they felt more accepting of themselves or more like themselves when they were walking. Many informants shared that they walked because they felt it was a part of their “therapy” or rehabilitation process, even though they were not actively participating in formal therapy at the time of the interviews. In contrast, some described how a power wheelchair or a manual wheelchair allowed them to maintain an element of their personality that they could not achieve with their walking capacity. Provided below are selected quotes from each informant to highlight how their individual perspectives on disability, self-perception, and self-presentation related to their mobility modes and devices.
“You know, I mean, you are injured, you want to feel normal, you want people to see you as, I guess, as disabled but still normal… The scooter, I think they feel I am more handicapped than when I am with the crutches.” [Informant 1]
“I am not disabled. I consider myself differently-abled because there is nothing, and I mean nothing, that I cannot do that you can do. It may take an assistive device to get something done but I can still do it. I was a fast walker before my injury. I was always in a rush to get where I was going. The power wheelchair lets me get so much done.” [Informant 2]
“…[I]t’s not really disability to me; it’s less ability, hindered ability, you-gotta-work-around-it ability. My therapists encouraged me to get a power chair and I told them no…I’m going to get fat and lazier, so I wanted a manual wheelchair…I think when I am walking, people are more, is that the right word, cognizant. They are more aware of my presence, I don’t know why.” [Informant 3]
“…[T]he power chair made me feel more handicapped. It was fun to shoot down hallways and roads with it, but other than that, it’s just not good. You are not really doing anything. You are just sitting there.” [Informant 4]
“…[R]iding around in a chair you know, is not well, it’s not normal. Wanting to be a member of the normal community, I guess, you know, physical normal community. You know, and I do not think of myself as a member of the disabled community.” [Informant 5]
“Normal people walk and people who are injured need to be in wheelchairs because they are injured. And I like to try to be as normal as possible. I just don’t like being at butt-level while everybody is standing.” [Informant 6]
“…[Using a wheelchair is] less fulfilling…. [I feel] less whole, if you will. Crutches represent my battle against my disability…They are a symbol of my independence and how hard I have worked. Sitting in a chair, the first thing people see when they see you, is not you, they see the chair, and they make a lot of assumptions when you are in a wheelchair. I know I am injured; I don’t need to be reminding everybody else all the time…I think that people see me coming with the crutches and they are less, I don’t want to say less uncomfortable, but they are less judgmental.” [Informant 7]
Informants further described how their perspective of disability, self-perception, and self-presentation evolved over time.
“..[I]t was very important for me right after my injury to be as, to get as far away as possible from being disabled…but you know later, I wasn’t quite as self-conscious anymore, maybe. Um, you know, or accepting, I guess. A little less angry.” [Informant 5]
“I didn’t have … [self-esteem] when I first got in the wheelchair. I was not sure of myself. I went through the why me’s, and the woe is me, and the everything you could think of. But I bounced back, and [it’s] what I think takes a lot of people a long time to do.” [Informant 2]
Every informant described the positive influence of interacting with others who had disabilities. The interaction with other individuals who also experienced disability provided support, which, over time, helped to shape their view of disability, self-acceptance, and strategies used for self-presentation relating to mobility modes and devices.
“…[B]eing at the fitness center seein’ that ok, I’m normal, everybody in here is normal, it’s the new normal.” [Informant 2]
“…Well, because you aren’t the only one who is busted and screwed up. They are busted, too. I get to hear other people’s problems.” [Informant 6]
Informants also expressed how their mode of mobility was associated with either a lack of awareness or over-awareness from others. Many informants felt that others were not as “aware” [Informants 1, 3, 7] of them when they were in a wheelchair. Informants expressed their inability to be at “eye-level” [Informant 1, 2, 5, 6, 7] when using a wheelchair, which not only reduced others’ awareness of them in the community, but also reduced their ability to interact socially. Informants also expressed a hyper-awareness from individuals in the community, noting that they frequently received offers for physical assistance when it was not required, particularly when walking.
Discussion
The results of this study offer the perspectives from individuals who are living in the community with motor iSCI, who have the capacity to walk and navigate community mobility decisions. This research study aimed to “give voice”33 to individuals with motor iSCI navigating community mobility choices in an effort to enhance patient-centered care. The insight gleaned from these informants’ narratives can help clinicians and researchers gain a deeper understanding of the unique challenges that individuals with iSCI encounter in relationship to community mobility mode and device choices. The results also provide a peer perspective for individuals with iSCI on the unique challenges of community mobility for individuals who experience disability from spinal cord injury.
One of the primary themes that emerged from this analysis resembles the classic model of motor control that attempts to explain and understand the complexity of the execution of a single movement.34 In this model, movement is described to emerge from the interaction of the task, individual, and the environment, where the individual must generate movement in order to meet the specific demands of the task in the environment in which it is performed.34 This motor-control framework is used to understand movement and to structure appropriate challenges for patients, as therapists devote significant time to retrain individuals with neurologic disease or injury in regaining functional movements. Interestingly, this analysis uncovered that informants structured their decisions considering the same elements as the already-established framework. However, informants considered how the interaction of these three factors (task, individual, and environment) would change over the course of the community outing, and their perspectives on disability further influenced their choices.
The recovery of walking abilities is a primary goal of individuals who have experienced a motor incomplete spinal cord injury3 and the positive effects of participating in walking training have been elucidated.35-39 But many informants of differing ambulatory capacity reported the use of both walking and wheeled mobility with differing devices, depending on the environmental circumstances, the task demands, and their body structure and function characteristics. Further, many informants utilized more than one mode of mobility during a single community activity.
Flexibility of Choice
All informants reported flexibility in how they navigated community mobility. This flexibility allowed them to accomplish the unique demands of a multitude of mobility-related activities. An analysis by Riggins et al40 explored quality of life factors and change in mobility status from inpatient rehabilitation to one-year post-spinal cord injury. Individuals who transitioned from primarily walking at discharge from inpatient rehabilitation to wheelchair use at one year post-injury had reduced quality of life, higher depression, and higher pain severity than those who maintained their mobility status or who transitioned from wheelchair use to walking.40 Although individuals who experience a spinal cord injury primarily want to pursue independent walking, these data should challenge clinicians to not view walking and wheelchair use as dichotomous choices. Instead, healthcare providers should encourage individuals to explore differing modes and devices for mobility to maximize flexibility, fluidity, and community engagement.
Economic Factors. There are, however, economic barriers that may limit the recommendation of having more than one device for community mobility. Many insurance companies will only pay for a primary device to navigate the home environment once every five years; that could have a considerable deductible.41 This would require individuals to cover both the cost of the deductible and the full expense of any additional device. Within this analysis, no informants described financial limitations in acquiring and maintaining their devices. This is a potential limitation of the study, as individuals that experience spinal cord injury have frequently been reported to experience a significant economic impact from sustaining the injury.42
Peers as Mentors
All informants expressed the comforting and supportive effects of peer relationships, which coincides with data from other published reports.27,43,44 However, for many newly-injured patients, the patient-to-patient peer relationship frequently involves another individual with little lived experience of disability. Many may still possess an inherently negative view of their disability, and may still be processing what they perceive as profound loss. Clinicians may consider connecting individuals with peers living in the community to support each individual in developing their own disability identity, free from the inherently limited abled lens.
Stigma and Acceptance
Informants expressed frustration with their perception of how the community viewed and interacted with them due to their disability. These informants’ frustrations echo a multitude of previous data describing similar feelings of stigma from individuals when navigating the community with physical impairments that lead to gait deviations, or with a wheelchair.25,45 The presence of this stigma contributed to how each individual thought about mobility mode and self-presentation. However, with greater experience of living with a physical disability, individuals’ perspectives evolved over time, and all described becoming more accepting of their physical disability, a perspective echoed in separate cohorts.24 This fruition of “acceptance” of disability warrants attention. Many of these informants were many years or even decades past their injury and still expressed an internal struggle with accepting their disability.
Disability advocates strongly admonish the notion that disability is a “burden” with resultant physical impairments inherently negative44 and the reduction of these impairments inherently good.43 Rather, disability scholars and advocates argue the issue lies in the environmental barriers and social perspectives that oppress individuals living with disabilities.44 And, unfortunately, the opinion that disability is fundamentally undesirable is still omnipresent in both the medical field and able-bodied population.46,47 This perspective should challenge rehabilitation clinicians and the medical community alike to evaluate their own perceptions of disability, and consider how they might influence their effectiveness as a healthcare provider. It is a moral imperative that each and every health care provider become “allies with persons with disabilities in the struggle to promote changes in the social environment”.48
Study Limitation
One notable limitation of this study is that those who were purposefully sampled were also active and engaged in the research setting, which may further limit translation to individuals living in the community with iSCI. Even though all effort was used to ensure saturation, individuals who participated in this analysis were closely involved with both the research and medical setting, and their perspectives may be reflective of the negative attitudes toward disability embedded in those environments. Further research should focus on quantifying each of the generated theory subcomponents to understand how each of them affect mobility choices.
Conclusion
The results of this analysis serve to recommend that rehabilitation clinicians expose individuals with motor iSCI to a multitude of mobility modes and devices, champion the development of peer-support programs within their healthcare and community environments, participate in deep self-discovery in inherent attitudes toward disability, and partner with individuals in the fight against disability discrimination in our healthcare systems and communities.
Affiliations
Carey L. Holleran, MPT, DHS, NCS1,2
Jennifer Fogo, PhD, OTR2,3
Stephanie A. Miller, PT, PhD, NCS2,4
- George Hornby, PT, PhD1,5,6
1 Program in Physical Therapy, Washington University in St. Louis, MO.
2 College of Health Sciences, Postprofessional Programs, University of Indianapolis, Indianapolis, IN.
3 School of Occupational Therapy, University of Indianapolis, Indianapolis, IN.
4 Krannert School of Physical Therapy, University of Indianapolis, Indianapolis, IN.
5 Indiana University School of Medicine, Department of Physical Medicine and Rehabilitation, Indianapolis, IN, USA.
6 Department of Physical Medicine and Rehabilitation, Northwestern University, Chicago, IL.
CLH – concept development, design, data collection/processing, analysis, writing
JLF – concept development, design, data collection/processing, analysis, critical review
SAM – analysis, critical review
TGH – critical review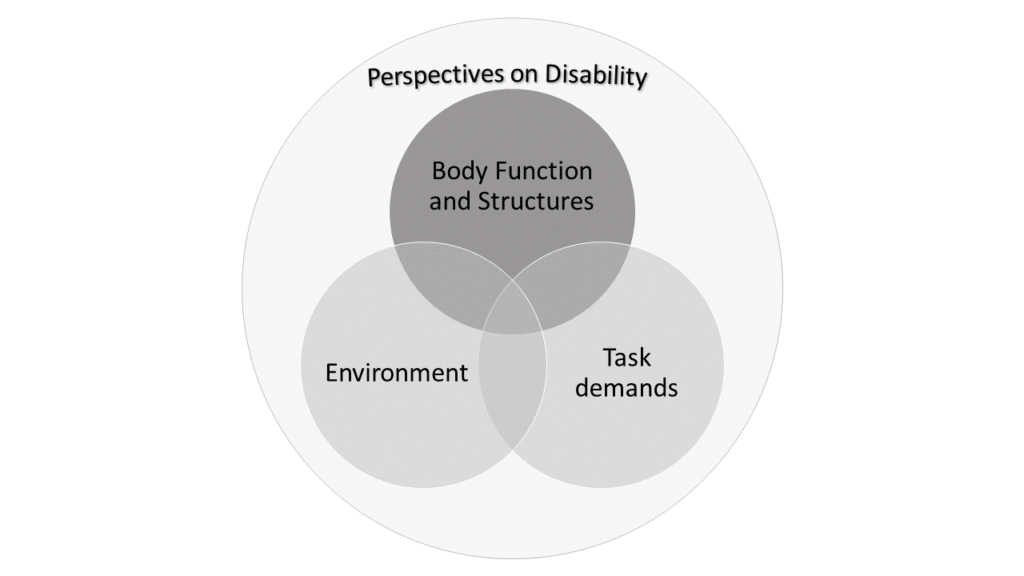
Figure 1. Interaction of the two primary themes depicting the iterative and ongoing analysis that each informant described when navigating community mobility method selection.
Table 1: Interview Question Guide.
Table 2. Demographic Information. Push-rim activated power assist wheels (PAPAW); UE (upper extremity); LE (lower extremity); Motor Scores from American Impairment Scale from American Spinal Injury Association (out of 50 points).
References
1. National Spinal Cord Injury Statistical C. Spinal cord injury facts and figures at a glance. J Spinal Cord Med. 2010;33(4):439-440.
2. Annual Report for the Model Spinal Cord Injury Care Systems B, AL. National Spinal Cord Injury Statistical Center. 2008.
3. Ditunno PL, Patrick M, Stineman M, Morganti B, Townson AF, Ditunno JF. Cross-cultural differences in preference for recovery of mobility among spinal cord injury rehabilitation professionals. Spinal Cord. 2006;44(9):567-575.
4. International Classification of Functioning, Disability, and Health: ICF [computer program]. Version 1.0. Geneva: World Health Organization; 2001.
5. Perry J, Garrett M, Gronley JK, Mulroy SJ. Classification of walking handicap in the stroke population. Stroke. 1995;26(6):982-989.
6. Saraf P, Rafferty MR, Moore JL, et al. Daily stepping in individuals with motor incomplete spinal cord injury. Phys Ther. 2010;90(2):224-235.
7. Waters RL, Adkins RH, Yakura JS, Sie I. Motor and sensory recovery following incomplete tetraplegia. Arch Phys Med Rehabil. 1994;75(3):306-311.
8. Crozier KS, Cheng LL, Graziani V, Zorn G, Herbison G, Ditunno JF, Jr. Spinal cord injury: prognosis for ambulation based on quadriceps recovery. Paraplegia. 1992;30(11):762-767.
9. Lapointe R, Lajoie Y, Serresse O, Barbeau H. Functional community ambulation requirements in incomplete spinal cord injured subjects. Spinal Cord. 2001;39(6):327-335.
10. Scivoletto G, Romanelli A, Mariotti A, et al. Clinical factors that affect walking level and performance in chronic spinal cord lesion patients. Spine. 2008;33(3):259-264.
11. Waters RL, Yakura JS, Adkins RH. Gait performance after spinal cord injury. Clin Orthop. 1993(288):87-96.
12. Kim CM, Eng JJ, Whittaker MW. Level walking and ambulatory capacity in persons with incomplete spinal cord injury: relationship with muscle strength. Spinal Cord. 2004;42(3):156-162.
13. Adams MM, Hicks AL. Spasticity after spinal cord injury. Spinal Cord. 2005;43(10):577-586.
14. Somers MF. Spinal Cord Injury: Functional Rehabilitation. Prentice Hall; 2001.
15. Chau L, Hegedus L, Praamsma M, et al. Women living with a spinal cord injury: perceptions about their changed bodies. Qual Health Res. 2008;18(2):209-221.
16. Benevento BT, Sipski ML. Neurogenic bladder, neurogenic bowel, and sexual dysfunction in people with spinal cord injury. Phys Ther. 2002;82(6):601-612.
17. Galvin RD. Researching the disabled identity: contextualising the identity transformations which accompany the onset of impairment. Sociol Health Illn. 2005;27(3):393-413.
18. Organization WH. Towards A Common Language for Functioning, Disability, and Health: ICF. Geneva, Switzerland; 2002.
19. Kaplan D. The definition of disability: perspective of the disability community. J Health Care L Pol. 1999;3:352.
20. Dibb B, Ellis-Hill C, Donovan-Hall M, Burridge J, Rushton D. Exploring positive adjustment in people with spinal cord injury. J Health Psychol. 2014;19(8):1043-1054.
21. Moin V, Duvdevany I, Mazor D. Sexual identity, body image and life satisfaction among women with and without physical disability. Sexuality Disabil. 2009;27(2):83-95.
22. Potgieter C-A, Khan G. Sexual self-esteem and body image of South African spinal cord injured adolescents. Sexuality Disabil. 2005;23(1):1-20.
23. Burns SM, Hough S, Boyd BL, Hill J. Men’s adjustment to spinal cord injury: the unique contributions of conformity to masculine gender norms. Am J Men Health. 2010;4(2):157-166.
24. Taleporos G, McCabe MP. The impact of physical disability on body esteem. Sexuality Disabil. 2001;19(4):293-308.
25. Bailey KA, Gammage KL, van Ingen C, Ditor DS. Managing the stigma: exploring body image experiences and self-presentation among people with spinal cord injury. Health Psychol Open. 2016;3(1):2055102916650094.
26. Baumeister RF, Hutton DG. Self-presentation theory: self-construction and audience pleasing. Theories Group Behav. 1987:71-87.
27. Jannings W, Pryor J. The experiences and needs of persons with spinal cord injury who can walk. Disabil Rehabil. 2012;34(21):1820-1826.
28. Glaser B, Strauss A. The Discovery of Grounded Theory: Strategies for Qualitative Research. Aldine de Gruyter; 1967.
29. Strauss C. Basics of Qualitative Research: Grounded Theory Procedures and Techniques. SAGE publications; 1998.
30. Strauss A, Corbin J. Grounded theory methodology. Handbook Qualita Res. 1994:273-285.
31. Henderson R. Appraising and incorporating qualitative research in evidence-based practice. J Phys Ther Educ. 2004;18(3):35-40.
32. Saunders B, Sim J, Kingstone T, et al. Saturation in qualitative research: exploring its conceptualization and operationalization. Qual Quant. 2018;52(4):1893-1907.
33. Jeffreys M. The visible cripple: Scars and Other Disfiguring Displays Included. New York: The Modern Language Association of America; 2002.
34. Schumway C WM. Motor control: Translating Research Into Clinical Practice. 3rd ed: Lippincott Williams & Wilkins; 2007.
35. Hicks AL, Adams MM, Martin Ginis K, et al. Long-term body-weight-supported treadmill training and subsequent follow-up in persons with chronic SCI: effects on functional walking ability and measures of subjective well-being. Spinal Cord. 2005;43(5):291-298.
36. Fuhrer MJ, Rintala DH, Hart KA, Clearman R, Young ME. Relationship of life satisfaction to impairment, disability, and handicap among persons with spinal cord injury living in the community. Arch Phys Med Rehabil. 1992;73(6):552-557.
37. Dijkers MP. Correlates of life satisfaction among persons with spinal cord injury. Arch Phys Med Rehabil. 1999;80(8):867-876.
38. Anderson CJ, Krajci KA, Vogel LC. Life satisfaction in adults with pediatric-onset spinal cord injuries. J Spinal Cord Med. 2002;25(3):184-190.
39. Hannold EM, Young ME, Rittman MR, Bowden MG, Behrman AL. Locomotor training: experiencing the changing body. J Rehabil Res Dev. 2006;43(7):905-916.
40. Riggins MS, Kankipati P, Oyster ML, Cooper RA, Boninger ML. The relationship between quality of life and change in mobility 1 year postinjury in individuals with spinal cord injury. Arch Phys Med Rehabil. 2011;92(7):1027-1033.
41. Your Medicare coverage. Available at: https://www.medicare.gov/coverage/durable-medical-equipment-coverage.html. Accessed January 5, 2017.
42. Merritt CH, Taylor MA, Yelton CJ, Ray SK. Economic impact of traumatic spinal cord injuries in the United States. Neuroimmunol Neuroinflamm. 2019;6.
43. Zola I. Disability statistics: what we count and what it tells us: a personal and political analysis. J Disabil Pol Stud. 1993a;42(167-173).
44. Gill C. Four types of integration in disability identity development. J Voc Rehabil. 1997;9:36-46.
45. Barbareschi G, Carew MT, Johnson EA, Kopi N, Holloway C. “When they see a wheelchair, they’ve not even seen me:” factors shaping the experience of disability stigma and discrimination in Kenya. Int J Environ Res Pub Health. 2021;18(8):4272.
46. Neville-Jan A. Encounters in a world of pain: an autoethnography. Am J Occup Ther. 2003;57(1):88-98.
47. VanPuymbrouck L, Friedman C, Feldner H. Explicit and implicit disability attitudes of healthcare providers. Rehabil Psychol. 2020;65(2):101-112.
48. Gray D, Hahn, H. Achieving occupational goals: the social effects of stigma. In: Christiansen C, Baum, C, ed. Occupational Therapy: Enabling Function and Well-Being. Thorofare, NJ: Slack; 1997.
Community Mobility Method Selection in Individuals With iSCI: A Qualitative Analysis
Carey L. Holleran, MPT, DHS, NCS; Jennifer Fogo, PhD, OTR; Stephanie A. Miller, PT, PhD, NCS; T. George Hornby, PT, PhD
A primary rehabilitation goal for individuals with motor incomplete spinal cord injury (iSCI) is to regain their walking abilities. But what factors influence their paths to achieving that goal? Although quantitative information may be readily available in the clinic, these authors note that there is a paucity of qualitative information detailing each individual’s personal choices regarding mobility methods. Through extensive interviews, this groundbreaking study presents a range of deeper factors to consider when working with an individual to achieve community mobility.
About the Author(s)

Carey L. Holleran, PT, MPT, DHS, NCS
Dr. Carey L Holleran, PT, MPT, DHS, NCS is an Associate Professor of Physical Therapy and Neurology and the Assistant Director of Student Assessment and Program Evaluation in the Program in Physical Therapy at Washington University School of Medicine in St. Louis. Dr. Holleran’s scholarship has focused on recovery after spinal cord injury and stroke and neurologic rehabilitation. Through many years of inpatient spinal cord injury clinical practice and research, she has developed a strong appreciation of how the humanities can influence clinical and research practices. She also values the importance of an explicit humanities curricula within DPT education.

This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.

